A stitch in time saves nine: Preventing and responding to the abuse and neglect of infants
You are in an archived section of the AIFS website
September 2009
Brigid Jordan, Robyn Sketchley
Download Policy and practice paper
Contents
- Introduction
- Infants involved in the child protection system
- A different approach to protecting infants
- Protecting infants from abuse and neglect using a public health model enriched by a human rights perspective
- Conclusion
- References
Introduction
My mother groan'd, my father wept;
Into the dangerous world I leapt,
Helpless, naked, piping loud,
Like a fiend hid in a cloud. (Blake, 1794/1982)
The idealisation of infancy in our culture is in part a defence against recognising the intense powerlessness, helplessness and dependency of the human infant (Bradley, 1989). Despite the fantasy of infancy as being a time of nirvana, the first 12 months of life pose the highest risk of death from homicide; the most frequent form being fatal abuse by a caregiver (Nielssen, Large, Westmore, & Lackersteen, 2009). This paper addresses many of the issues confronting Australia at present: how to ensure the protection of individual infants (aged 0-3 years), how to respond to infants who have suffered neglect or abuse in ways that alleviate their suffering and heal and protect them from further harm, how to create a society that reduces the risks of infants and children becoming subject to neglect and abuse, and how to deal with the limits and failures of such endeavours.
The particular focus of this Issues paper is child abuse and neglect in infants aged 0-3 years. Infants are a harbinger of hope within their individual families and at a societal level. The public health model has particular appeal because of its focus on preventative efforts, the underpinning societal recognition in Australia that all new families need some support, and the wish of individual families and the wider society to prevent intergenerational transmission of vulnerability and disadvantage. A children's rights perspective can help keep the focus on the subjective experience of infants, and their rights to health, happiness, social participation and relief from pain and suffering.
In this paper, we commence by discussing the over-representation of infants in child protection services, the vulnerability of infants and infancy as a foundational developmental stage for later outcomes. The way in which a public health model enriched by a human rights perspective might inform service delivery to protect infants from abuse and neglect is explored. Finally, as the most difficult area of practice for protecting infants is out-of-home care, detailed attention will be given to some of the key challenges for protecting and caring for infants removed from their families.
Infants involved in the child protection system
The age distribution of children involved in child protection services within Australia indicates that infants are one of the primary client groups of child protection services. In 2007-08, 44.7% of all verified cases of child abuse and neglect and 42% of all children admitted into care involved an infant aged 0-4 years (Australian Institute of Health and Welfare [AIHW], 2009). Infants' physical fragility and almost total dependence on others to meet their needs means that they are also the group most vulnerable to fatal abuse. The Victorian Child Death Review Committee (2008) reported that of all deaths of children known to child protection services between 1996 and 2007, 63% (129 of 204) were infants under 3 years and 33% (68 of 204) of all child deaths were infants under 6 months. Similarly, in New South Wales, homicide of infants aged less than one year was higher than rates among older children and adults, and most child homicides were the result of physical abuse (Nielssen et al., 2009).
These data are consistent with research showing that, compared to older children and adolescents, the vulnerability of infants places them at a disproportionate risk of death, serious injury or developmental delay resulting from abuse or neglect (Butchart & Phinney Harvey, 2006; Larrieu, Heller, Smyke, & Zeanah, 2004).
Infants, because of their particular vulnerabilities, require an immediate response to child protection reports or notifications. However, the need for tertiary level intervention can be reduced by a service system that values primary prevention and health care models and encourages and supports vulnerable families earlier, in order to be able to provide optimal outcomes for infant development. This approach is consistent with current directions in service system reform in Australia (Council of Australian Governments, 2009). Given the innate vulnerability of infants and the fact that infants are the largest client group (by age) of child protection services, there is a need for services to actively address the specific needs of infants and young families. For more information on the vulnerability of infants, see Box 1.
Box 1: The vulnerability of infants
The particular vulnerability of infants arises from their almost complete dependence on others for survival, their physical immaturity, under-developed verbal communication, and their social invisibility. Because the first few years of life set the stage for all that follows, infancy holds the greatest risk of harm, but it also holds the greatest opportunity for positive change or successful intervention.
Infant development
Infancy is a time of rapid physical, cognitive, language, social and emotional development. Thus infants are extremely vulnerable to the effects of maltreatment or deprivation (Melmed, 2004). Brain development begins in utero, but the brain is only about 25% of adult size at birth. In the next three years, the brain grows to 90% of adult size and develops the connections between nerve cells (Royal Australian College of Physicians, 2006). Although inherited genetic potential predisposes an individual to develop certain abilities, skills and characteristics, environmental influences determine the ultimate expression of these potentials in all the domains of development - cognitive, language, social and emotional (Siegel, 2001; Stevenson, 2007). Future development beyond the infancy period is based on experiences and relationships in the early years (Melmed, 2004). These early experiences affect physical health (Royal Australian College of Physicians, 2006), emotional regulation (including the stress response system) and mental health across the life course, cognitive development, learning and the capacity for full engagement and participation in and thus access to social resources (e.g., education, employment, relationships).
Attachment relationships and infant development
The attachment relationship between an infant and their primary caregiver has a profound impact on the infant's current functioning and future development. Attachment theory has much to offer in understanding the effect of abuse and neglect on infants, the features of services needed at a secondary intervention level and best practice from the infant's point of view at the tertiary level of child protection, including the provision of safe and emotionally enriching, quality out-of-home care.
Feeling secure, loved and having a safe base to explore from and return to are ongoing needs met by the parent-caregiver relationship within all societies, although specific attachment beliefs, values and practices of parents and caregivers will differ across cultures (Reebye, Ross, & Jamieson, 2008). The attachment relationship between an Aboriginal infant and their caregiver, for example, may be influenced by their historical, cultural and spiritual contexts (Humphreys & Kiraly, 2009; Yeo, 2003).
An attachment figure (usually the mother) is a person with whom the infant has an ongoing relationship, to whom the infant turns and experiences as a source of safety, comfort and care and who, in turn, is emotionally attuned to the infant. Sensitive and responsive care-giving builds a secure infant-parent attachment relationship and promotes the conditions for optimal behavioural, social and emotional development, including a greater capacity for emotional regulation, positive social interactions and better coping skills. Interactions within the relationship need to be nurturing, protective, secure and consistent in order for infants to feel confident to explore their environment and to have the psychological resources available for learning.
Over the first few months of life, infants form attachment relationships with additional people with whom they have an ongoing relationship and whom they experience as a source of safety and nurturing (e.g., father, grandmother, babysitter). These relationships are in a hierarchy and will be sought by the infant in hierarchical order, according to their availability when the primary caregiver is not available (Bowlby, 1969, 1980; Brisch, 2004). Infants' capacities to develop these new relationships are enhanced when they have a secure attachment relationship with their primary caregiver.
Attachment relationships can be characterised as secure, insecure (i.e., either avoidant or ambivalent but organised) or disorganised (see Table 1). A disorganised attachment relationship is among the greatest indicators of developmental and protective risks for the young child (DeBellis, 2001), with this pattern of attachment relationship being frequently seen in maltreated and clinic samples. Unsurprisingly, research has demonstrated that up to 82% of maltreated infants suffer from serious disturbances of attachment with their caregivers (Carlson et al., 1989).
| Attachment style | Caregiver responses | Infant behaviour |
|---|---|---|
| Secure | Sensitive, responsive, consistent, attuned, reliable (e.g., prompt comforting when infant distressed, warm interested response to infant's wish to communicate or play, empathy and acceptance of infant's point of view) | Able to regulate emotions, seek help from others when distressed, adaptable to changing circumstances and able to explore their world |
| Insecure (avoidant) | Connected enough to protect the infant, but minimises the importance of attachment issues, can be dismissive of infant's attachment cues, insensitive to infant's signals and emotional needs | Shows little distress on separation, and minimal joy when reunited with caregiver, over-regulation of affect, avoidance of emotional intimacy and defensive focus on exploration |
Insecure (ambivalent) | Inconsistent or unpredictable emotional availability and response to infant's attachment behaviours and emotional needs (e.g., at times over-protective or over-stimulating and at other times rejecting or ignoring) | Overly engaged with attachment figure and may feel too anxious about caregiver's emotional availability to freely explore the environment |
| Disorganised | Unresponsive, intrusive, hostile or violent (these parents may have experienced trauma themselves) | Chaotic and confusing behaviour (e.g., hyper-vigilant, freeze or fear when parent appears, dissociative behaviours) |
Impact of trauma, violence and neglect on infant development
At a subjective level, infants can suffer distress, emotional and physical pain and overwhelming fear or terror in response to sudden separations, experiencing neglect, being assaulted or witnessing violence. Experiences of neglect and abuse can undermine the infant's basic sense of trust in the world. Hill and Solchany (2005) noted that infants are especially vulnerable and powerless, as they cannot request help when they feel threatened or unsafe.
Exposure to trauma (e.g., abuse, neglect, exposure to violence) affects every dimension of an infant's psychological functioning (i.e., emotional regulation, behaviour, response to stress and interaction with others) (Perry, 2002). Very young infants may be overwhelmed with intense negative emotions, manifesting in incessant crying, inability to be soothed, feeding problems, sleep disturbances, hyper-arousal and hyper-vigilance, and intense distress during transitions. Toddlers may experience intense separation anxiety, wariness of strangers, social avoidance and withdrawal, and constricted affect and play. They are likely to have reduced tolerance of frustration and problems with emotional regulation evident in intractable tantrums, non-compliance and negativism, aggression, and controlling behaviour. Extreme anxiety may be expressed as new fears, constricted and repetitive play, hyper-vigilance, reckless and accident-prone behaviour, and fear of body damage. Toddlers may regress and have somatic complaints (Drell, Siegel, & Gaensbauer, 1993; Zeanah & Sheeringa, 1996). These traumatic responses can lead to unmanageable stress in the infant-parent relationship (Lieberman, 2004).
The recognition and understanding of infants' subjective experiences of and response to traumatic experiences is crucial in order to ensure that services provided at both the secondary and tertiary intervention levels are designed to meet a traumatised infant's need for the relief of immediate suffering and to prevent long-term impacts, including intergenerational impacts.
For many children living in vulnerable families, multiple risks converge to compromise safety and development. This is particularly apparent in cases of neglect and emotional abuse - the most common forms of maltreatment substantiated by child protection services in Australia (AIHW, 2009). Chronic stress caused by multiple adverse circumstances and events accumulates and can damage the developing brain (Bromfield, Gillingham, & Higgins, 2007), the effects of which are more pronounced in infancy and early childhood (Shonkoff & Phillips, 2001). The importance of cumulative harm in child protection was first recognised in Victoria with the inclusion in the Children, Youth and Families Act 2005, s 10(3)(e), of the requirement for practitioners to consider the effects of cumulative patterns of harm on a child's safety and development. Similar legislation and policies have since been developed in other Australian jurisdictions.
A different approach to protecting infants
Australia is facing an overloaded child protection system, with increasing reports to child protection services and placements of children in out-of-home care (O'Donnell, Scott, & Stanley, 2008). The majority of reports to child protection services are not investigated (53%) or substantiated (82%), and many of the children and families involved do not receive services (AIHW, 2009; Bromfield & Holzer, 2008).
Scott (2006) argued that there are many risks associated with an overloaded child protection system, including:
- superficial assessments or premature case closures, resulting in children in serious jeopardy remaining unprotected;
- problems in vulnerable families escalating and becoming entrenched;
- the likelihood that families who have been notified but not substantiated being further alienated from services due to shame, fear and stigma, resulting in their problems escalating or becoming entrenched and subsequently requiring child protection involvement;
- the need to redirect scarce resources to investigation, which reduces the resources available to provide casework services for children already in out-of-home care (e.g., working towards reunification, placement support, addressing health and educational needs); and
- an erosion of the child protection workforce due to high levels of stress, resulting in high staff turnover and staff shortages.
It is recognised that there will always be a need for "coercive" and "deterrent" tertiary services to provide timely treatment to children who have been abused and for high-quality, stable out-of-home care placements for children who cannot live at home (O'Donnell et al., 2008). However, there is also increasing recognition of the need for alternate approaches to reducing the pressure on overloaded child protection systems, such as placing a greater focus on prevention and diverting all but the highest risk cases away from child protection services (Council of Australian Governments, 2009).
The profile of child protection service clients raises issues about what the best model (or mix of models) is for conceptualising and delivering child protection services. It has been argued that a public health model is a "way forward" for child protection in Australia. Advocates of this model argue that it offers an alternative to meeting the current crisis in Australia of an overloaded child protection system (O'Donnell et al., 2008; Scott, 2006). However, a limitation of a public health approach is that the subjective experiences of individual children can be lost. Reading et al. (2008) proposed that a human rights perspective can enrich public health and protective responses to child abuse and neglect.
Public health model
The public health model takes a population approach to health promotion and disease prevention. The focus of this approach is on the identification and response to the underlying causes of health problems, which requires statistics on the prevalence of a health problem and ongoing measurement of the problem to determine the effectiveness of interventions (O'Donnell et al., 2008; Reading et al., 2008).
The application of a public health approach to child abuse and neglect emphasises providing services at the population level in order to foster healthy children, families and communities (e.g., the Communities for Children Strategy, see Edwards et al., 2009). However, a public health approach recognises that prevention is not always effective and there is a need for coercive (i.e., child protection) interventions (Council of Australian Governments, 2009; O'Donnell et al., 2008). Thus, the essential elements of service provision under a public health model applied to child abuse and neglect are:
- the use of universal services for children and families as a "platform" for preventing neglect and abuse (primary);
- the provision of specialist services addressing specific risk factors that compromise parenting in vulnerable families (secondary); and
- the protection and treatment of children who have experienced abuse and neglect, including statutory child protection services (tertiary) (O'Donnell, et al., 2008).
To date, the application of a public health approach to child protection has focused on service system reform and investment in primary and secondary services (Bromfield & Holzer, 2008). However, a limitation of the public health approach as it has been applied to child abuse and neglect in Australia is the lack of national prevalence data to establish the magnitude of the problem and enable measurement of change.
The model of primary, secondary and tertiary preventions and interventions is visually represented as a pyramid (Bromfield & Holzer, 2008) in Figure 1, which lists examples of services that specifically target infants.
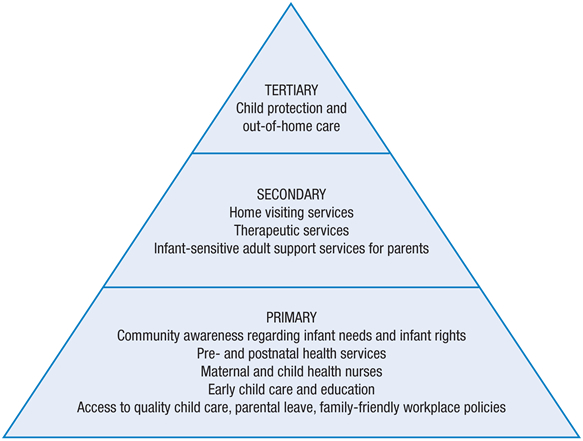
Source: Adapted from Bromfield & Holzer, 2008
Figure 1. Diagrammatic representation of a public health model for infants
Human rights perspective
A human rights perspective emphasises rights of participation and provision as well as protection (Reading et al., 2008). Public health and rights-based approaches to child abuse and neglect have similar goals and point to similar interventions; however, a rights perspective is concerned with children as a group as well as the individual child, risks are seen as the responsibility of the state, and the child's right to call on the state is acknowledged (Reading et al., 2008). Fundamentally, a human rights perspective, underpinned by the United Nations Convention on the Rights of the Child (United Nations, 1989), views child maltreatment as a violation of children's rights (Reading et al., 2008).
Protecting infants from abuse and neglect using a public health model enriched by a human rights perspective
In this section, the potential contribution of a public health model towards the protection of infants will be discussed in terms of policy and practice issues arising at the level of primary, secondary and tertiary service provision (see Figure 1). While this paper uses the public health model categorisation of primary, secondary and tertiary interventions, it is noted that there are some limitations to this classification system. Depending on the experiences of children and families, a single service (e.g., a home visiting program) may be experienced by one family as a secondary intervention preventing abuse and neglect and by another as a tertiary intervention responding to family problems to prevent re-abuse (Bromfield & Holzer, 2008). Implementation of this dual perspective of public health and human rights at a policy level will involve difficult decisions about relative resource allocation between primary, secondary and tertiary services, and challenges the community to consider how much we are prepared to pay for the prevention of child abuse and neglect.
Primary preventative interventions
Social infrastructure provision
From a human rights perspective, all children have the right to experience the conditions for optimal health, growth and development, and society has an obligation to ensure that parents have the necessary resources to raise children (Reading et al., 2008). Child protection activity is typically concentrated in families and neighbourhoods experiencing the greatest level of poverty and poverty-related factors such as unemployment, poor health, poor education and high crime (Bromfield & Holzer, 2008; Victorian Child Death Review Committee, 2008).
Income security, stable and secure housing in safe neighbourhoods, accessible and affordable health care, and opportunities for social engagement are key elements of social infrastructure provision in a primary prevention model (Centre for Community Child Health, 2009; Higgins & Katz, 2008; Reading et al., 2008; Royal Australian College of Physicians, 2006). Social policies that encourage mothers to stay home with their infants beyond the first few months (e.g., paid parental leave) lead to better health outcomes (Center on the Developing Child at Harvard University, 2007). This social infrastructure increases the emotional and financial resources available to parents for child rearing.
Universal services and health promotion
Pregnancy and birth is a key transition point for all families that presents both an opportunity for hope and change, and increased stress on families. Universal services aim to relieve some of this stress and are intended for the whole community. They need to be accessible, culturally sensitive and well-promoted in order to reach those who are most vulnerable. Examples of primary interventions for infants include: pre- and postnatal care (including maternal and child health nurses), child care and early childhood education, and healthy infant development promotion campaigns.
Pre- and postnatal care and maternal child health nurses
Maternal and neonatal outcomes are often worse for women and infants from low socio-economic, vulnerable or socially isolated groups (Schmeid et al., 2008; Wilensky & Prosser, 2008). Continuity of care during pregnancy and labour improves the maternity experience for women, improves health outcomes and reduces obstetric intervention rates. However, in Australia women may encounter numerous maternity care providers, making their experience of care fragmented. Concerns have also been raised about the decline in breastfeeding rates and the increased rates of postnatal depression in Australia, and it has been suggested that this may be associated with shorter hospital stays and fragmented community services (Department of Health and Ageing, 2008). These stresses are likely to have greater impact on mothers and infants facing other social risks.
Maternal and child health nurses can play an important role in supporting new families, as they are potentially in a position to identify infants who are at risk and provide some support to families, including referral to secondary services. They can also assist with infant development and health issues, coordinating new parent groups and developing partnerships with other service providers to support new families. There are, however, some significant challenges in using universal maternal and child health nurse services to identify families in need of secondary preventative services. A UK study found that in the first 4 months of an infant's life, health visitors only identified 47% of the families who were later referred to social work services as being in "high need" (Wright, Jeffrey, Ross, Wallis, & Wood, 2009). "Universal" health services may not in reality be equally available or may not be accessed by those who need them most (Schmeid et al., 2008).
Perhaps an untapped resource in Australia is the general medical practitioner (GP). Infants and families in difficulty tend to initially present with a "physical" complaint (e.g., infant crying or feeding problems) to a universal primary health service. A Victorian study found that by the age of 1 year, infants averaged 10.9 visits to a general practitioner and 14.3 visits to a maternal and child health nurse (Goldfeld, Wright, & Oberklaid, 2003). These primary health settings offer an enormous early opportunity to provide families with anticipatory guidance, and for early detection and intervention for infant-parent relationship problems. GPs may be especially well positioned, as they may be providing care for parents' issues that are known risk factors for child maltreatment, such as mental illness or substance abuse. However, the availability of GPs (especially those able to bulk bill), appropriate training and funding for inter-professional collaboration, and providing indirect care to the patient (e.g., attending case conferences) remain challenges. A Victorian survey found that in the previous month, half of the GPs seeing families with infants had no contact with the local child and family health nurse, but that 88 % of those who did found it to be helpful both to their practice and to the mother (Mbwili-Muleya, Gunn, & Jenkins, 2000).
Early child care and education
High-quality, developmentally informed early child care and education is a potential resource for all families. The key features of high-quality child care are warm, responsive and caring adult-child relationships, consistent and secure care with continuity of staff, individualised curriculum, high infant-caregiver rations, small group sizes, a language rich environment, and highly skilled, trained and experienced caregivers who receive ongoing staff development (Center on the Developing Child at Harvard University, 2007; Centre for Community Child Health, 2008). Some of this can be achieved by regulation and standards, but other aspects (such as continuity of staffing) require a community commitment to ensuring there are appropriate salaries and carer structures for workers in the early child care sector.
Early child care and education services are a frequently untapped resource for children at risk. They can function as a secondary preventative intervention by ameliorating aspects of social disadvantage and deprivation (e.g., providing compensatory experiences, including relationship experiences, not available at home), reducing exposure to at-risk home environments, and providing some respite from child care responsibilities for overburdened parents. It has been argued that the "patchwork" of early childhood services involving many departments at all three levels of government in Australia means many children miss out on these services (Centre for Community Child Health, 2008). Some families may not be able to access child care for their infant due to social isolation, cultural and linguistic diversity and/or lack of knowledge or understanding of child care systems. For example, only 16% of preschoolers enrolled in one family support program for vulnerable families accessed any early child care or education services, and many did not attend free kindergarten services (Children's Protection Society, 2007).
Health promotion strategies
Population-based strategies such as health promotion campaigns can be used to target particular risks (e.g., the impact of maternal smoking and alcohol intake on the unborn child) and create a climate of recognition and valuing of infant rights. Reading and colleagues (2008) noted the importance of the community embracing the principles and spirit of the Convention on the Rights of the Child and gave the example of how both the outlawing of physical punishment of children and a campaign to change public attitudes to violence against children reduced child maltreatment in Sweden. There has recently been increased public awareness of the physical vulnerability of infants (e.g., don't shake the baby campaigns), infant emotional and social development, the emotional impacts of trauma, and infant memory, cognitive and reasoning capacities. Such awareness could lead to an increased sensitivity to, awareness of and empathy for infants' subjective experience, and also more realistic expectations in terms of infants' emotional needs, capacities to regulate behaviour and to learn.
Secondary preventative interventions
Secondary preventative interventions may be embedded in universal services (e.g., targeted maternal and child health home visiting services, such as the South Australian Nurse Family Home Visiting program that provides home visiting to mothers with risk factors). Adult-focused services that tackle specific risks and disadvantage faced by parents may be able to become secondary preventive services by expanding their mandate and role to include a focus on the needs of the infant and the infant-parent relationship (O'Donnell et al., 2008).
Family support services have a long tradition of offering services to vulnerable children and families. In Victoria, the Child FIRST program offers vulnerable families earlier, more intensive support to address their problems before they escalate and require child protection involvement. Child FIRST teams take referrals from concerned professionals and others, assess the needs of the family and then link them into the appropriate services. The help received might include maternal and child health services, child care and preschool, parent support groups, school holiday programs, household management, as well as home support and basic health and educational support for children.
There is a need for specialist services - especially infant mental health services that address problems in emotional and behavioural functioning and disturbances in infant-parent relationships - to be readily available to vulnerable infants and families, both before these difficulties escalate and also as a tertiary therapeutic service when the infant has been exposed to neglect, abuse or trauma.
It has been argued that insufficient availability of secondary preventative family support services is one of the drivers for an overloaded child protection system in Australia (Bromfield & Holzer, 2008). When there is insufficient supply to meet demand, agencies may start to "gate keep" in ways that seem innocuous but have the effect of excluding the very families who most need and would most benefit from the service (e.g., by requiring families to telephone the agency to make an appointment or complete intake forms).
Home visiting and family support services
Currently, there are many models for home visiting and family support services and they differ in the degree to which they target the functioning of the whole family, parents' concerns, parenting issues or the infant-parent relationship.
There is evidence of the effectiveness of some home visiting interventions in preventing child maltreatment (Butchart & Phinney Harvey, 2006; MacMillan et al., 2009). Key features of successful home visiting programs for infants and families are: well-trained and supervised professional staff who deliver programs with clear goals, with a focus on infant behaviour and relationships, and of sustained duration (Center on the Developing Child at Harvard University, 2007; Olds, 2006). Early and intensive support by skilled home visitors when vulnerable families are expecting their first child is recommended (Center on the Developing Child at Harvard University, 2007) and has been implemented in South Australia. A critical element in successful home visiting interventions is the development of a therapeutic relationship between the professional and the infant and family. Many high-risk families do not seek to actively engage with support services because of their own traumatic attachment history and ensuing lack of trust in "helping" agencies. Fraiberg and Shapiro (1980) highlighted the need to attend to parents' internalised model of attachment (i.e., the relationship they had as children with their own parents) when establishing a casework relationship.
Specialist early childhood care and education programs for at-risk infants and children
There may be limits to what can be achieved for vulnerable children through universal early child care and education services. There is still debate about how much non-parental child care is too much, and long hours of care may not be in the best interests of young vulnerable infants. There is a risk that the availability of full-time child care may lead to a very young infant remaining at home when their best interests would be served by out-of-home care (i.e., foster or kinship care). The National Institute of Child Health and Human Development (NICHD) study of early child care found that increased time in non-maternal care was associated with increased externalising behaviour problems, regardless of the quality of care or maternal sensitivity (NICHD Early Child Care Research Network, 2003). The significance of these findings has been debated, with one research centre arguing that the effect size of the amount of child care is small and affects a minority of children (Center on the Developing Child at Harvard University, 2007). These are issues that warrant serious consideration in considering how to meet the needs of infants at risk of abuse and neglect.
A number of intensive programs (e.g., the Carolina Abecedarian Project or the Perry Preschool Program) have demonstrated sustained benefits for disadvantaged children into their adult years. A review of Early Head Start programs in America found the most powerful effects were evident in programs that combined centre-based and home-based services, enrolled parents during the pregnancy and served children at medium risk (Center on the Developing Child at Harvard University, 2007). Victoria's Children's Protection Society (2007) proposed a model for an integrated specialist therapeutic child care and education program and family support service, informed by attachment and trauma theory, and with individual infant case planning. This has the potential to meet the particular needs of infants who are at risk of abuse and neglect as well as those in out-of-home care who need additional support to compensate for their early deprivation and traumatic experiences. The characteristics of this integrated service model are: small group sizes (perhaps multi-age), primary caregiver assignment, low staff-to-child ratios (no more than two children to one carer in the first year of life), continuity of care, and flexible centre-based attendance combined with in-home child care scheduling around individual infant or toddler needs. Together, they have the potential to provide vulnerable infants with a predictable, nurturing and responsive interpersonal environment that will facilitate all facets of development, particularly emotional and social development.
Reviews of innovative home visiting or early child care programs point to the need for programs to be well designed, theoretically informed, and faithfully implemented. It has been noted that "scaling up" is always a major challenge (Center on the Developing Child at Harvard University, 2007; O'Donnell et al., 2008). Another issue emerging is that no one program is a "magic bullet", especially when families have multiple risk factors present. In an innovative program in Miami that combined court and therapeutic services and had an Early Head Start program linked to the drug dependency court, evidence-based parenting classes had to be modified several times in order to have any impact on the parenting behaviour of substance-using parents (Dice, Claussen, Katz, & Cohen, 2004).
Infant mental health services
Specialist infant mental health services - like specialist early child care and development services - have the potential to function as both secondary and tertiary preventative services. From a rights perspective, infants should have access to mental health services in their own right from the time of onset of the earliest signs of disturbances in infant emotional regulation (persistent crying, sleeping, feeding problems), or infant-parent relationship problems where these do not respond to parenting education, advice or support by primary health care workers. From a public health or cost-benefit perspective, intervening early in the life of the problem may prevent mental health and social functioning problems and costs to the community later in life.
Assessment and treatment services for infant mental health problems need to target the infant symptoms, the infant's emotional development and infant-parent relationship, including trans-generational issues that may be undermining the health of the infant-parent relationship.
The developing attachment relationship between an infant and parent may be distorted by a parental history of unresolved losses or traumatic life events (including parent's own history of childhood neglect or abuse). Specialised services can reduce any escalation of distress (infant crying can be a proximal cause of shaken baby syndrome and fatal child abuse in extreme family situations; Barr, Trent, & Cross, 2006) and disturbed attachment relationships.
Attachment relationships influence how the children of today parent the next generation (Leckman & Mayes, 2007). Infant mental health interventions have the potential to reduce some of the risk factors that can evolve in the next generation, such as poor parenting history and poor emotional regulation (which in turn may lead to mental illness or substance abuse) (Fonagy, 1998; Lieberman, Van Horn, & Gosh Ippen, 2005). Although treating maternal depression alone does not in itself improve outcomes for infants, mother-infant relationship-focused treatments can ameliorate the negative consequences of maternal mental illness on the developing infant and increase the mother's sensitivity towards their baby (Fonagy, 1998; Fraiberg & Shapiro, 1980; Nylen, Moran, Franklin, & O'Hara, 2006; Poobalan et al., 2007; Seligman, 1994).
According to the Center on the Developing Child at Harvard University (2007), infant mental health treatment can reduce the immediate distress of infants and toddlers suffering from withdrawal, depression or a traumatic stress response as a result of abuse or neglect, as well as stop the trajectory of long-term negative impacts due to hyper-vigilance, hyper-arousal, avoidance and associated lack of engagement with learning environments. Access to infant mental health services is especially important for infants in out-of-home care. Maltreatment and the often repeated separations from caregivers means that infants and toddlers who are placed in out-of-home care are at increased risk of mental health disorders. Exclusion of disruptive or extremely distressed children from child care, an increasing number of prescriptions for emotional/behavioural problems for preschoolers and the high incidence of postnatal depression underline the need for infant mental health services.
Current service delivery issues include the fact that many child and adolescent mental health services (CAMHS) find it hard to prioritise infants for services when they have a large caseload of disruptive older children and adolescents. Some services will not accept a relationship disorder as a referral problem, as it is a dyadic problem rather than a psychiatric entity in the child. Australian governments have increased investment in mental health services for infants and mothers; however, this is usually through the gateway of perinatal mental health services and thus services are accessed through the mental health vulnerability of the mother rather than symptoms in the infant, the infant-parent relationship, or another vulnerability (e.g., substance use, family violence, maternal history of child abuse).
There is also a need for infant-focused mental health services in neonatal and paediatric wards in hospitals. Many of the infants whose deaths were reviewed in the Victorian Child Death Inquiry were born prematurely, some with complex medical needs and multiple disabilities, and many came from families where there were issues - such as family violence, substance use and mental illness - that impair parenting capacity (Victorian Child Death Review Committee, 2008). It is likely these infants had long hospital admissions. Such admissions represent a missed opportunity to engage parents in a therapeutic relationship, to more fully assess the attachment relationship and to intervene and repair that relationship. Of concern are the infants in similar circumstances who fortunately did not come to the attention of the Child Death Review Committee but still carry this vulnerability and compromised mental health and wellbeing.
Adult-focused support services
Within a preventative intervention framework, services at the secondary level (see Figure 1) would also require adult support services to encompass the wellbeing of the infant and to consider the impact of specific vulnerabilities on parenting capacity and the infant-parent relationship as part of its mandate and service provision (O'Donnell et al., 2008). Many services for adults focus on the needs of their adult clients and don't consider that their role could include ensuring the safety and wellbeing of the infants who are in the care of their adult patients (Cousins, 2005). There is a need for specialised training to educate adult workers about infant needs and capacities (e.g., capacity for memory and traumatic stress responses), and to develop the skills to be able to screen for emotional and developmental problems of infants. In addition, many services for adults (e.g., drug treatment services) are not "child-friendly" and therefore parents are deterred from accessing them. Dawe, Harnett, and Frye (2008) argued that many child protection issues could be prevented if drug and alcohol services could provide discrete services for parents. There may also be challenges for workers in keeping infants' rights in mind in a service that has adult needs as the primary focus (Cousins, 2005).
There are risk factors for children and families that are common across the lifespan, including: parental mental illness, alcohol and drug abuse, disability or complex needs, family violence, family history of child protection intervention, infant/child health issues and social isolation. Some risk factors have a particularly heightened significance for infants: prenatal alcohol and drug use, maternal mental illness, parental intellectual disability and adolescent mothers. The infant-caregiver relationship is often compromised by these risk factors, especially when they impact on the parents' capacity to not only provide a safe environment, but one that is nurturing and consistent for the infant. From a child rights perspective, Reading and colleagues (2008) have argued that some family vulnerabilities, such as parental substance abuse or parental intellectual disability, can result in social exclusion, which results in children's participatory rights also being infringed. For more information about parental risk factors, see Box 2.
Family violence services have the potential to incorporate an assessment of infant and mothers' needs into their service provision and also facilitate referral to secondary and tertiary services that address the infant's trauma response and the impact of violence on the mother-infant relationship (e.g., the Peek-a-Boo Club, Bunston, 2008). Universal service provision is important here too; access to affordable, secure, dignified housing; secure income support; and affordable, high-quality child care will assist mothers to leave violent partners to protect themselves and their children.
Larrieu and colleagues (2004) found that an accumulation of risk factors, rather than any one specific risk factor, was most important in predicting the loss of custody of infants to the child protection system. Multiple risk factors have a cumulative and exponential rather than a simple additive impact on the infant. New models of care (perhaps an infant case worker/advocate) have the potential to address infant needs across the "silos" of different adult services.
Box 2. Parental risk factors
Parental vulnerabilities (risk factors) may place infants at risk of abuse or neglect. These are discussed in some detail in this section, as adult-focused services can only function as a secondary preventative intervention service if specific risks to the infant are addressed in program design and implementation.
Parental substance misuse
Prenatal maternal addiction to alcohol and/or other drugs can result in still births and low birth weight, as well as congenital anomalies (including foetal alcohol syndrome), physiological addiction, and severe developmental problems in the infant (Mrazek, 1993; Zuckerman & Brown, 1993). There is evidence that the foetus may experience periodic withdrawal symptoms in utero and those infants of women who use opiates during pregnancy may be born addicted to the drug (Householder, Hatcher, Burns, & Chasnoff, 1982), putting them at high risk of neonatal abstinence syndrome at birth. Neurobiological problems occurring in infants exposed to alcohol and/or other drugs prior to birth include difficulties with attention, memory, problem-solving and abstract thinking (Shonkoff & Phillips, 2001).
Post-birth, substance dependence affects parenting capability in many ways and high rates of child maltreatment have been reported in families with parental substance misuse (Dawe, 2007). When substance-affected or suffering withdrawal, parents may struggle to provide adequate supervision, attend to the infant's physical care, or be responsive and attuned to their emotional and interactive needs (Dawe et al., 2008).
Parents who misuse alcohol and other drugs are also generally more likely to suffer from mental illness, including depression, low self-esteem, anxiety, eating disorders, self-harm and suicide attempts, and this places infants at a greater risk of abuse and neglect because all facets of the infant-parent relationship and infants' environment are adversely affected under these conditions (Dawe, 2007; Smarsh Hogan, Myers, & Elswick, 2006).
Maternal and/or paternal mental illness
There are many different types of mental illness, each of which may affect parenting in a different way. The key mental health problems include depression, schizophrenia, bipolar disorder and borderline personality disorder. In general, the effects of parental mental illness on infant development include: the increased risk for infants to develop mental health problems themselves, the increased risk of infants experiencing psychosocial stress, poverty and family discord, and the increased risk of insecure attachments (Seifer & Dickstein, 1993). In many cases, mental illness can cause the parent to withdraw, lack emotional engagement, be less responsive and more negative (Newman & Stevenson, 2005; Seifer & Dickstein, 1993).
Severe mental illness involving hallucinations and delusions or fixed beliefs about the baby may put the infant at risk of serious harm, including violence or abuse and, sometimes, death (Sved Williams, 2004). If a parent lacks insight into their illness or has trouble coping with the side effects of medication, symptoms may remain untreated or poorly controlled and the parent may remain delusional, disorganised and unable to care for the infant. Mothers with Borderline Personality Disorder have a core disturbance in their sense of self, and experience disordered personal relationships, variable changes in mood, disturbed thinking patterns and significant self-harm (Sved Williams, 2004). They may be fearful of abusing their infants and so become withdrawn, or alternatively they may feel an intense need to protect and so appear intrusive and anxious (Newman & Stevenson, 2005). In addition to these issues, environmental risks such as social disadvantage and social isolation (which are often associated with mental illness), or protective factors such as having a supportive other parent or care provider, will also have an effect on infants' developmental outcomes (Sved Williams, 2004).
Parents with intellectual disabilities
Infants of parents with intellectual disabilities are at risk of neglect, due to their parents' skill deficiencies and stress (Feldman, 2004; Feldman & Léger, 1997), and data from New South Wales show that they are more likely to be made wards of the state (Llewellyn & McConnell, 2003). Such parents may be especially unable to flexibly respond to the infants' changing needs, putting the infant at risk of neglect. However, there are great variations in parenting skill levels and family circumstances. Parents with intellectual disability may struggle to cope if their infant has special needs (Gilberg & Geiger-Karlsson, 1993). It has been argued that parents with intellectual disabilities who abuse their children may share similar predisposing factors as adults who do not have an intellectual disability, including: history of childhood deprivation, low self-esteem, poor interpersonal skills, stressful family relationships and social isolation (Dowdney & Skuse, 1993). While researchers may not agree as to whether it is the intellectual disability that causes child abuse and neglect, or the accompanying socio-economic difficulties faced by many of these families, it is generally agreed that greater support is required for parents with intellectual disability and their infants to decrease the risk of harm (Booth & Booth, 1993; Dowdney & Skuse, 1993; Feldman, 2004; Feldman & Léger, 1997; Llewellyn & McConnell, 1998, 2003). There is very little research on the subjective experience of infants and children who grow up with both parents having intellectual impairment.
Adolescent mothers
Most adolescent mothers do not abuse their children, but the infants of adolescent mothers are at a higher risk of parent-child relationship problems and neglect (Carter, Osofsky, & Hann, 1991). An Australian study found that 60% of pregnant adolescents were identified as having a major social or psychological problem adversely affecting their ability to carry out daily activities of living (including parenting activities), and the consumption of drugs and alcohol was higher than that reported for the general adolescent Australian population (Quinlivan, Peterson, & Gurrin, 1999). Studies have found that adolescent mothers talk less to their infants and frequently have difficulty interpreting infant cues or articulating the feelings of their babies (Carter et al., 1991; Osofsky, Hann, & Peebles, 1993), all of which affect infant development and the infant-caregiver attachment relationship. However, it is worth noting that home visiting programs have been found to be effective for young parents, particularly in assisting young mothers to re-engage with education (Sweet & Appelbaum, 2004).
Parents of infants with poor health (special needs)
Premature or medically fragile infants and those with genetic or other congenital abnormalities can suffer from poor health effects associated with low birth weight; feeding, settling and sleeping difficulties; prolonged and frequent crying; and developmental delay, and they may have complex medical needs. All of these factors, in addition to long hospital stays, confinement in an incubator and loss or separation experienced by parents (Brisch, 2004; Fegran, Helseth, & Fagermoen, 2008) have an impact on the relationship between infants and their parents. Mothers who are not able to hold, feed or perform other caregiving tasks due to the medical fragility of their infants may find it difficult to feel a strong bond with their baby. Parents may experience significant grief and loss associated with not having the anticipated "normal" baby, and they may also place blame on themselves, the infant or others for the infants' illness. These perceptions will affect their ability to relate to and care for the infant unless they are well supported through this painful time.
The vulnerability and care needs of a sick or disabled infant increases the stress experienced by parents and if they do not have the support or emotional, social and financial resources required to manage this stress, the infant's risk of neglect or abuse is heightened. The social gradient of health (i.e., poorer health status being associated with lower socio-economic status [Commission on Social Determinants of Health, 2008]) means that a premature or sick infant is more likely to come from a family with other vulnerabilities (Parslow, et al., 2009).
Family violence
Intimate partner violence perpetrated against women frequently occurs during pregnancy. The 2005 Personal Safety Survey found that 36% of all women who reported violence by a previous partner reported that violence had occurred during pregnancy (Australian Bureau of Statistics, 2006), often with severe physical consequences, including miscarriage (Taft, Watson, & Lee, 2004). A baby in the womb will experience the adverse effects of any violence perpetrated on their mother, which can have a negative impact on development (Klein, Gilkerson, & Davis, 2008). Humphreys, Houghton, and Ellis (2008) concluded that violence during pregnancy is a serious form of child abuse and that the "risks posed by these perpetrators to both women and the unborn child need to be taken extremely seriously" (chap. 2).
Post-birth, family violence continues to pose a serious risk to infants. A review of child homicides in New South Wales revealed that men were responsible in 57% of cases of infant homicide. Most of these men were not mentally ill, and domestic violence was a factor in many of the families involved (Nielssen et al., 2009). The authors highlighted the importance of responding to domestic violence and threats against women and their children. In terms of parenting, the physical and psychological impacts of violence on mothers may affect their parenting, particularly their emotional availability and ability to be attuned to the infant's needs. Partner violence towards a mother has also been conceptualised as an attack on the mother-child relationship (Humphreys, 2007).
From the infant's perspective, people, sensations, images, situations and places may all act as traumatic reminders or triggers for those who have experienced abuse or neglect. In partner violence, the infant witnesses the parents as victim and aggressor and is unable to rely on either of them for their own protection and comfort. Given this scenario, it is likely that specific aspects of the parent's behaviour, tone of voice, body movement and facial expressions may become traumatic reminders for the infant (Lieberman, 2004).
Tertiary preventative interventions
Tertiary interventions are needed to provide an immediate and long-term response in order to keep an infant safe from imminent or further neglect or abuse, alleviate the infant's suffering and reduce the long-term harms of neglect and maltreatment that have occurred. These services include statutory child protection services, the courts, and out-of-home care. In this domain, coercive and deterrent measures may be necessary (O'Donnell et al., 2008) and the use of a children's rights perspective that keeps the best interests of the infant in the forefront is helpful.
Although at times referred to as a "last resort", child protection and out-of-home care services are at times required as a "first resort" in situations of serious risk. Recent policy and legislative changes in Australia's eight state and territory child protection systems that specifically apply to the protection of infants include the introduction of reporting unborn children in NSW, Victoria and the ACT.
Judicial services
Child protection issues confront societies with important questions of values and the balance between the protection of children and the rights of parents to autonomy and privacy (Reading et al., 2008). It has been contended that the adversarial nature of Australia's legal system may not be ideal for ensuring children's rights to protection from abuse and neglect (Allen Consulting Group, 2003).
A recent innovation in Florida, USA, has been the establishment of infant/toddler court teams. In this model, the judge partners with a child development expert to create a team of child welfare and health professionals, child advocates and community leaders to provide services to the abused or neglected infants. The court teams were established to address the co-occurrence of child maltreatment, substance abuse, parental mental illness and family violence, and have resulted in system reforms, increased sharing of resources across agencies and collaborative strategies (Zero to Three, 2006). A key element of this model is a monthly review meeting of all the individuals and organisations providing court-mandated services in order to review the progress of the case, and enabling the judge to focus on the infant's healing while adjudicating the case. In this model, all infants, toddlers and mothers receive assessment services and selected mother-infant dyads are referred to a parent-infant therapeutic intervention. The model has led to improved outcomes in health care and developmental screening services, a reduction in placement instability and moves, an increase in parent-child visits (prior to the new model the frequency was less than once a week) and an increase in kinship placements (Zero to Three, 2006).
Child protection
Challenges facing child protection systems that directly impact on outcomes for infants include: the increased number of notifications placing pressure on the system; more resources being used for investigation and assessment instead of prevention and early intervention; recruitment and retention of a skilled workforce; and the need to "break down silos" between government and non-government agencies (Bromfield & Holzer, 2008). Retention of a skilled and trained workforce is especially important for infants at risk of abuse and neglect. One report found that a single change in caseworkers reduced the likelihood of a child receiving timely permanency planning by 52% (Walker & Youcha, 2006). As undergraduate health and welfare professional courses often do not focus on infant development in the curriculum and many workers will not have worked with normal healthy infants (unlike the nursing or medical profession), there are large gaps in knowledge and understanding of infant development and the infant-sensitive practice that is required to work with families and infants to ensure their safety and wellbeing. To ensure quality service provision and prevent burnout, child protection workers need specific support and reflective supervision (Zero to Three, 2004).
Out-of-home care
An infant's immediate safety (physical and emotional) is paramount, and his/her immediate or long-term best interests may require temporary or permanent removal from the care of parents. There has been little published work of an empirical or clinical nature on the subjective experience of infants in out-of-home care. Infants are the fastest growing category of children entering care (AIHW, 2009). Some out-of-home care is provided by family or others known to the child (kinship care), while for other infants the care is provided by a stranger (foster care) (Richardson, Irenyi, Kelleher, & Horsfall, 2009). In some countries, foster carer is seen as a professional activity and carers are paid a wage, whereas in Australia it is primarily a voluntary activity (McHugh, 2003). The degree of support and training offered to foster carers varies enormously.
Practice challenges in the provision of out-of-home care
Foster parent role and expectations
Many foster parents encounter an inherent role conflict. On the one hand, the infant needs them to be a primary attachment figure, to be emotionally available, preoccupied with the infant and their needs, and committed to them. However, until a permanent plan of reunification with parents or permanent placement is made, the potential duration of this relationship is unknown. The foster parent is facing the issue of loss while simultaneously forming an attachment with the infant. While many excellent foster carers are able to manage the challenges of caring for a newborn or infant in these circumstances, many others may struggle. They may become emotionally "burnt out" from a history of caring for many infants who have then left their care and the implicit temporary nature of the foster care relationship. At times, expectations and norms about the foster carer's role can undermine the relationship with the infant (e.g., treating an infant in one's care as one would treat one's own child may be seen as undermining the role of the biological parents and a violation of the limits of the role of the out-of-home carer). In fact, research evidence demonstrates that infants require the commitment of foster carers to establish an attachment relationship with them in order to thrive. In a study of 84 caregiver-child dyads, it was found that commitment (defined as the extent to which the carer had a strong emotional investment in and was motivated to have an enduring relationship with a particular child) was the strongest predictor of placement stability (Dozier & Lindhiem, 2006).
Developing an emotional connection with a traumatised infant
In cases where infants suffer from severe attachment disturbances resulting from abuse and neglect, the infant's response to separation from the parent, their particular expression of loss, grief reactions and distorted attachment behaviours may make it difficult for the foster parent to provide sensitive and responsive care (Dozier & Lindhiem, 2006; Goldsmith, Oppenheim, & Wanlass, 2004). To ensure healing for the infant and the stability of the placement, there is a need for foster carers to receive ongoing training and reflective supervision that is focused on how to read the infant's emotional cues, how to develop an emotional connection with a traumatised infant, how the infant's experience of maltreatment and/or prior placement disruption may be impacting on them, and how the foster parent may need to adapt their own intuitive parenting style to accommodate the response of the particular infant (Melmed, 2004).
Health care needs of infants in out-of-home care
The Royal Australian College of Physicians (2006) has highlighted issues in health care provision for children in out-of-home care. These children have high rates of acute and chronic health problems and developmental disabilities, which placement in out-of-home care does not automatically remedy. The college recommends routine health screening and assessment of all children entering alternative care, the formulation of a health plan that includes attention to mental health, enhanced care management and treatment services, access to health records of birth parents, enhanced communication with birth parents and foster parents and improved support and training for foster carers. Multiple placements and changes in caseworkers can make it hard for a coherent medical history of the infant to be obtained; resource shortages discourage routine screening and assessment; and access and cultural safety issues may make it hard for kinship carers to access mainstream health services. Research has demonstrated that foster carers and social workers under-report psychological problems of children in care (Royal Australian College of Physicians, 2006). This may be because they have little professional contact with normal healthy infants growing up in emotionally robust families and further underlines the need for careful reflective supervision and support, along with routine health checks.
Infant contact with parents while in out-of-home care
Once an infant is placed in out-of-home care, there are practice dilemmas for the courts and child welfare practitioners that challenge even experienced practitioners. Many of these practice issues revolve around the central dilemma of ensuring that the infant is provided with a secure attachment and caregiving relationship with someone who is not their parent, while simultaneously working to ensure that the best possible circumstances are provided for the infant to have an ongoing meaningful relationship or to be united with their parents where this is in the infant's best interests.
Placement in out-of-home care is a time of stress and major adjustment for the infant. While there is likely to be relief from the overwhelming stressors of neglect or abuse, the separation from parents is often sudden, possibly traumatic. A difficult experience or experiences has precipitated the placement (Walker & Youcha, 2006) and placement may involve the loss of known supportive figures in the infant's world, such as grandparents, neighbours or child care workers.
Visits with biological parents can both facilitate the continued attachment relationship between infants who have been removed from their parents' care or the establishment of a relationship for infants who have never been in the care of their parents. Smariga (2007) suggested that parental contact:
promotes healthy attachment and reduces negative impacts of separation for the child and parents, establishes and strengthens the parent child relationship, eases the pain of separation and loss for the infant and parent, keeps hope alive for the parents and enhances parents' motivation to change, involves parents in their child's everyday activities and keeps them abreast of the child's development, helps parents to gain confidence in their ability to care for their child and allows parents to learn and practice new skills, provides a setting for the caseworker or parenting coach to suggest how to improve parent child interactions, allows foster parents to support birth parents and model positive parenting skills, provides information to the court on the family's progress (or lack of progress) towards their goals, facilitates family assessments and can help the court determine whether reunification is the best permanency option for the child, helps court decide if reunification best option, helps with the transition to reunification. (p. 6)
From a child rights' perspective, it could be argued that visits with parents should provide a benefit and not incur physical or emotional costs or risks for the child.
Current practice in many jurisdictions in Australia does not meet these conditions. The potential benefits of parent-child contact will not automatically eventuate as a result of face-to-face contact alone. The infant's subjective experience will depend on a myriad of factors, including whether parents were ever the primary caregiver for the infant, the quality of interactions prior to removal, the distress involved in separation from the foster parent for the duration of the visit, and the likelihood of the infant returning to live with their parents. Smariga (2007) argued for frequent, safe and high-quality contact, but described visiting as a "conditional" right of parents and children. Because the infant-parent relationship is often unhealthy prior to placement, the visits should be regarded as a planned therapeutic intervention that offers an opportunity to heal a damaged relationship, and therefore to be resourced and evaluated with this framework in mind. It has also been argued that the goals of contact should be clearly articulated for each individual child and family (Gauthier, Fortin, & Je Liu, 2004). The best outcome for infants would be ensured by visits being supported by an assessment of and skilled therapeutic intervention to heal the infant-parent relationship. Such an approach would provide relationship-building and emotional support for the child and parent during the visit; ongoing assessment of progress and the demands on the infant; re-appraisal and reworking to a realistic and safe schedule if the infant is distressed by the visits or the parent does not attend; and reviewing according to developmental stage, emotional development and the dynamics of the infant's relationships with both the caregiving family and the parent. Visits should cease if there is a danger that parents will physically or psychologically harm the child or if the visits are extremely traumatic for the child (Smariga, 2007).
Both the name and models of parent-child contact bear further consideration. It has been suggested that naming the contact "family time", "family access" or "family interaction time" could keep the focus on the quality of the relationship and therapeutic goals. Alternative models of contact include therapeutic visitation where infants and parents meet with an infant-parent psychotherapist, supervised visitation centres, and foster placements where the parent and child are placed together (often adolescent mothers) (Smariga, 2007).
One of the most contested current issues is how frequent contact with parents should be for very young infants in out-of-home care. A Victorian study reviewed the case files of all infants in care who were under one year of age. Thirty-four per cent had court-ordered high-frequency contact (defined as four to seven visits per week); however, these visits occurred at this frequency in only half the cases. The most common reason for lack of visitation was parents being unable to maintain such a schedule of high-frequency visiting due to their life circumstances (Humphreys & Kiraly, 2009). This study found that high-frequency visiting schedules were not associated with increased rates of reunification with parents one year later (23% of high-frequency contact and 22% of low-frequency contact infants were reunited with one or both of their parents one year later).
The literature usually argues for "frequent" (not defined) contact to preserve or build attachment relationships and ease the emotional pain and grief that the infant experiences in separation from the only caregiver they have known (Goldsmith, et al., 2004; Smariga, 2007). In Australia, contact orders can involve up to seven days a week of visiting with parents, with the infant being transported up to an hour in each direction by a worker (or several different workers across the week). Commentators (e.g., Goldsmith, et al., 2004; Smariga, 2007) arguing for frequent contact often contextualise their comments with a statement about how visits may be limited to one hour a week or a month.
Attachment theory is appropriately invoked to explain infants' needs for ongoing contact with their parents. However, Bowlby (1969) also drew attention to the way in which attachment behaviours and exploratory behaviours are complementary, as infants cope with novel or stressful experiences and learn from the supportive presence of their primary attachment figure (secure base). If feeling overtaxed or stressed, attachment behaviours (clinging, crying) escalate and exploratory behaviours shut down. From this perspective, the arrangements for infants to visit their parents need to ensure that the infants are feeling as secure as possible, alert, awake and happy in order for them to have the curiosity and emotional energy to invest in getting to know and to interact with their parents. This is especially true if the parents have never been the primary caregiver for the infant.
Attachment theory articulates how infants need a continuous, emotionally available and secure primary attachment relationship and it is the robustness and security of this relationship that enables them to develop multiple attachments. If the arrangements for visits undermine the infant's relationship with their current carer, or are undertaken in conditions that do not ensure the infant has access to someone in their hierarchy of attachment figures available to help them regulate their emotions and behaviour, visits may in fact undermine the very goal they are trying to achieve (i.e., eventual reunion with the parents or meaningful relationship with them while the child is in out-of-home care). Arrangements that undermine the infant's trust in the foster carer and do not support the best possible interaction with parents during visits run the risk of leading to placement breakdown, and blunting of the infant's capacity to develop trusting relationships with anyone.
Infants have a hierarchy of attachments, so it may be that high-frequency access is important in the early stages of out-of-home care while the infant mourns the loss of primary caregiver/parent (if that is what they were) and forms a relationship with and learns to trust the new carer. The optimal amount of contact after the initial transition to placement may well depend on what "costs" are involved in the visit (separation from new carer, lack of attachment figure during transport, disruption to sleep, play and other daily routines), and if there is distress in interactions with the parents (mis-attuned interactions, parents fighting with each other during the visit, etc.). The whole issue of quality of time versus frequency and length of time for visits needs careful thought. Many people advocate for less frequent, longer blocks of time for the infant and parent to spend together, but the infant's subjective experience of such arrangements depends on the age of infant, their capacity for self-regulation, and the quality of interactions with their parents. A long block of time with parents means a longer block of time away from their secure base attachment figure (foster parent). It is worth remembering that infants growing up in the community with their parents, where there are no protective concerns, develop secure attachment relationships with grandparents and family friends over time on contacts as infrequent as once a week or less.
Potential benefits of visits between infants and their parents are likely to be undermined by three current practice issues: breaks in the continuity of experience with the primary carer, transport arrangements, and disruptions to the infant's daily routines (Humphreys & Kiraly, 2009).
Breaks in continuity of experience with foster or kinship carers
In the first few weeks and months of life, babies are still developing the capacity for emotional regulation and self-soothing and are highly reliant on the sensitive and emotionally available presence of their carer (Brazelton & Cramer, 1990). Most can only tolerate brief periods of separation from their primary caregiver. This is especially true if a baby's capacity for self-regulation is compromised in any way (e.g., by being medically fragile, suffering withdrawal from opiates at birth, or having persistent crying or feeding difficulties). In these instances, the baby's own body might be experienced as being unpredictable and they are especially reliant on the continuous predictable responses from their caregiver to be not so frightened and to develop confidence that they will get over their upset. This process of interactive emotional regulation and the development of emotional security has usually already been severely disrupted by the neglect or maltreatment that has led to the infant being placed in out-of-home care. It is critical that visiting schedules do not involve unmanageable separations from the foster carer that will undermine that developing relationship and cause emotional distress or further traumatise the infant.
Transport
From the infant's point of view, the period of time of being transported to a visit with parents can be a "no man's land" between the experience of being with their foster carer and their contact with their parents (which may be reassuring, evocative of painful feelings of loss or distressing, which depends on the quality of the relationship prior to entering care and the nature of ongoing interactions). In jurisdictions where foster parents do not transport infants to or accompany infants during the visits with their parents, the infant's subjective experience while being transported to and possibly during the visit can be an experience of emotional abandonment. Unless the caseworker accompanying the infant is known to the infant and is sensitive and responsive, the infant is left to their own emotional resources to manage the emotions evoked by separation from their carer, being accompanied by an unknown adult, travel, reunion with parents, interaction with parents, separation from parents, travel home again with unknown adult, and reunion with their foster carer. This is not optimal for relationship-building and if arrangements involve multiple handling by multiple people within a day or over a week, then visits are likely to be highly stressful, counterproductive and, in fact, damaging.
Disruption to infant's daily routine
Infant visits to parents may be scheduled around agency needs (availability of staff to transport infant, practicalities of infants visiting in the morning to ensure afternoon slots are available for school-aged children, etc.) rather than being determined by the individual daily timetable of the infant. This reduces the potential benefit of visits, as the infant is likely to have their own biological rhythms disturbed in order to be put in the car and thus is less likely to be in the alert and calm state that promotes quality interaction with and responsiveness to parents during the visit. For example, when an infant is woken from their sleep to be taken to a visit, they are likely to arrive tired and cranky, they may be fed whether a feed is due or not, and the infant may become so overwhelmed that they fall asleep to cope with the visit, which is unsatisfying for both infant and parents.
The relationship between frequency of visits and reunification
One of the main arguments for frequent contact between very young infants and their parents is to preserve the attachment relationship and thus enhance the possibilities of reunification. Research has shown that the relationship between frequency of contact and reunification is complex (Biehal, 2007; Humphreys & Kiraly, 2009). Although some studies have found a high correlation between higher frequency contact and reunification, the relationship may not be causal. Biehal (2007) found that contact was only one explanatory variable for reunification; other factors, such as low threshold for entry into care in the first place, were also important. It is possible that, in Victoria, the availability of services such as Child FIRST means that the threshold for taking infants into out-of-home care is quite high and thus frequent contact is not associated with higher rates of reunification. Biehal also cautioned against assuming that reunion is, of itself, a good outcome for children in out-of-home care and cited a study in Wales that found that 31% of infants less than 12 months old who had been returned to the care of their parents were re-abused or neglected after their return home.
Should visits sometimes be ceased?
From a children's rights perspective, there may be circumstances in which the infant has a right to not have any contact with parents or to have very infrequent limited contact. The literature that argues for frequent contact usually acknowledges that there may be circumstances where visits should be ceased (e.g., if there is a risk that parents will physically or psychologically harm the child or if the visits are extremely traumatic for the child) (Smariga, 2007). However, from a children's rights perspective, a more nuanced approach may be needed, especially if it is considered that visits with parents should provide a benefit to the infant and not incur physical or emotional costs or risks.
The parent as a traumatic reminder
When parents have assaulted an infant, the mere presence of the parent has the potential to be a traumatic reminder. Infants can remember experiences from birth; memories are encoded and recalled perceptually (implicit memory) and not through conscious processing as with verbal memory. Particular states of mind in an infant (e.g., fear or terror) can be encoded as an implicit form of memory and these states of mind can be reactivated in the presence of the abusive parent (Lieberman, 2004; Siegel, 2001). Specific aspects of the parent's behaviour, such as voice, body movement or facial expression, can be a traumatic reminder that signals danger to the infant that an attack is imminent (based on past experience this is a realistic automatic appraisal by the infant) (Lieberman, 2004). In these circumstances, the infant's subjective experience is of being reminded and terrified of the terror and pain of abuse. Visits in these circumstances are likely to cause emotional suffering, hyper-vigilance, and effects similar to the impact of the original abuse. These dangers are heightened when the visits occur without the infant having their primary caregiving adult (foster parent or kinship carer) present. From a children's rights perspective, assumptions about the benefits of having contact visits for infants who have been assaulted by their parents need careful examination.
Infants' rights in respect of the quality of the contact visits also need to be addressed. The secondary preventative interventions that are possible when visits are conceptualised as a therapeutic intervention were discussed earlier. Exposure to a hostile, substance-affected or thought-disordered parent, or witnessing violent exchanges between parents and workers may also be harmful to the infant.
Over the last twenty years, "still face" experiments and experimental work on neonatal imitation have demonstrated infants' capacity for primary inter-subjectivity (awareness of the feelings and motives of others) and their distress when the "rules" of reciprocal communication were broken. In these experiments, mothers were asked to interact normally with their 6-week-old infants and then to hold a blank face for several seconds. The infants initially tried harder to engage their mothers with vocalisations but quickly became distressed (looked away, started to pull at their ears, etc.) These experiments demonstrated that infants are inter-subjective beings from the beginning, and rely on sensitive and responsive interactions for their emotional wellbeing (Murray, 2006). Constant misreading of an infant's cues and misattributions of an infant's intent within an interaction are a significant source of stress for the infant. If this is the quality of the visit, then the potential benefits of visits are unlikely to accrue without specialised therapeutic intervention that changes these interactions. If visits continue to be characterised by hostile or rejecting interactions, despite intervention, then the infant has a right to the cessation of visits.
More recent developments in neuroscience research, particularly the discovery of "mirror" neurons as the intention-detection centre of our brains, highlight infants' capacity to detect and be affected by the state of mind of the person with whom they are interacting (Meltzoff & Brooks, 2007; Stern, 2008). Thus, being in the presence of a very disturbed, hostile, harsh, belittling or vengeful adult will have an emotional impact on the infant even if they do not understand the verbal content of what is being said. Although the term "psychopath" has dropped out of favour (Seabrook, 2008), a proportion of adults who abuse their infants will be psychopaths who show no remorse, are without empathy and engage in premeditated abuse. Visits with a parent like this are likely to be extremely disturbing and damaging for an infant.
From a tertiary prevention perspective, visiting arrangements for infants need to ensure that the infant is not further harmed, has the best chance of recovery from abuse and neglect and can participate fully in life now and in the future. The optimal visiting arrangements for infants who will never return to live with their parents is a complex issue.
When reunification is unlikely
Factors that indicate a poor prognosis for reunification include when a parent has previously killed or seriously harmed a child, when a parent has repeatedly harmed a child with pre-meditation, when parents are entrenched in a drug culture and have demonstrated no significant effort to change and when another child has been involuntarily removed from a parent's care (National Clearinghouse on Child Abuse and Neglect Information & National Adoption Clearinghouse, 2005).
Concurrent permanency planning
Evidence presented by Shonkoff and Phillips (2001) on the neuropsychological effects of attachment relationships demonstrates a child's need for security, nurturing and continuity in attachment relationships in order to develop optimally. The need for sensitive caring and stable relationships is especially crucial for infants who have been neglected or abused (Melmed, 2004). This research supports permanency planning for infants and children in the child protection system. Infants may not be able to afford the time to wait for their parents to recover from risk factors such as mental illness or drug addiction when these seriously impair parenting capacity. Even if parents do overcome their difficulties, from a human rights perspective, the best interests of the child means that reunification should not be a "prize for parent's rehabilitation" (Gauthier et al., 2004). It is still a common misconception that (especially younger) infants are "resilient" and can manage moves from one foster carer to another when they haven't spent much time with them (e.g., when foster parents go on holiday) or that the infant can manage moves between home and foster care. However, the disruption of attachment ties with foster parents is likely to constitute a severe trauma that reinforces feelings of abandonment with short-term reactions such as anxiety, sleeping disorders, angry outbursts, destructive behaviours and denial of affect (Gauthier et al., 2004; Goldsmith et al., 2004; Melmed, 2004). With each disruption comes progressively more difficulties in managing the stress of transition. With each loss, the capacity to adapt and adjust to new challenges is compromised, as is the capacity to develop trusting relationships.
The need to ensure stability in the life of infants and reduce the number of placements has led some to argue for concurrent rather than sequential planning (Walker & Youcha, 2006). Concurrent planning refers to case management that comprises a family reunification case plan being pursued, while at the same time developing an alternate plan for permanent care. If the case goal changes, the alternate plan is already in place. Concurrent planning is designed to reduce case drift and to give children stability as early as possible (Frame, Berrick, & Coakley, 2006).
Parents relinquishing care
From a tertiary prevention perspective, child protection services need to support parents to address the loss, grief and other emotional reactions involved in coping with being unable to care for their infant, the infant's placement in out-of-home care being involuntary, and any intergenerational issues involved in their lack of capacity to parent. It is also important to ensure that the infant's visits with them are meaningful. Failure to address these issues is likely to reduce parents' capacity to cooperate with concurrent planning. It may also result in the birth of a replacement child, in which case there is a risk that the trauma of abuse and neglect, removal and placement, and contested court cases will be re-enacted.
Service collaboration and links between primary, secondary and tertiary services
The promise and challenge of using a public health model for the prevention of child abuse and neglect is that it requires action across many areas of government at all three tiers (Commonwealth, state/territory and local governments), cooperation between government and non-government sectors, and linkages between primary, secondary and tertiary level services. It has been argued that strong collaborations across the sectors of health, education, housing, employment, community-based agencies and social services would be most effective in the prevention of both child abuse and neglect and/or the recurrence of child protection notifications for families at risk (Australian Infant Child Adolescent and Family Mental Health Association, 2004; Blakester, 2006; DePanfilis & Zuravin, 1999; Scott, 2006). In the UK, mechanisms for facilitating inter-agency collaboration have been mandated in the Children's Act 2004.
This comprehensive, multi-level and holistic approach often also seems very difficult to achieve in practice at the individual case level. Child death review committees have noted that effective case management requires concerted cooperation and coordination when children are involved in multiple services (Commission for Children and Young People and Child Guardian, 2008; Department of Health and Human Services, 2007; Victorian Child Death Review Committee, 2008). For example, in 2008 the Queensland Child Death Case Review Committee recommended that consolidated case management processes be developed to address instances where a child's case involves multiple government and/or non-government agencies (Commission for Children and Young People and Child Guardian, 2008). The recommendation emphasised identification of children with complex cases or multiple needs and that services to these children be coordinated to ensure child-focused practices are not compromised (Commission for Children and Young People and Child Guardian, 2008). In another example, the Victorian Child Death Review Committee (2008) observed that there had been insufficient case planning meetings and hospital discharge meetings, which may otherwise have increased the capacity of services to exchange critical information, clarify roles, develop appropriate plans and perhaps save infant lives. Often, initial case planning meetings that did occur did not have a follow-up meeting scheduled. This means that case drift could occur or agencies were not aware when another agency concluded their service or had a change in staff. Thus, a case plan that when drafted was best practice in meeting the needs of an infant and family could become derailed when a component part (e.g., the drug counselling) is no longer available.
If adult-focused secondary preventative services expand their canvas to include the needs of the infant and the infant-parent relationship, then collaboration with child protection services will need to include regular planning and case goal discussion, with clearly defined roles for service providers. When services aim to work collaboratively with each other, it is important to keep all stakeholders "in the loop" and to constantly monitor and assess the treatment goals and outcomes for infants. This is important for addressing the predictors of recurrence of child maltreatment and neglect, which can be ameliorated by secondary services such as family stress, partner abuse, lack of social networks, and the interaction between family stress and the lack of social supports (DePanfilis & Zuravin, 1999). The therapeutic court teams model trialled in Florida may offer a model for ensuring good service collaboration that succeeds in addressing risk factors (Dice et al., 2004).
Conclusion
In this paper, we have explored the issues involved in applying a public health approach together with a human rights perspective to healing and protecting infants at risk of abuse and neglect. Australia is well placed, given its platform of universal health and welfare services, to embrace change in its approaches at the primary, secondary and tertiary levels of intervention. Possibilities include enriched primary health and welfare services, health promotion campaigns, specialist early child care and education programs, an expanded infant-sensitive focus for adult-based support services and increased access to infant mental health services. A rights-based perspective also requires the social investment and commitment to those infants who have been harmed by abuse and neglect to ensure that their rights take precedence over parents' rights. Ultimately we are aiming to minimise the negative impacts of abuse and neglect on infants and facilitate their best possible developmental outcomes and opportunities for full participation in society into the future.
References
- Allen Consulting Group. (2003). Protecting children: The child protection outcomes project. Melbourne: Department of Human Services.
- Australian Bureau of Statistics. (2008). Personal Safety Survey, Australia, 2005 (reissue). Canberra, ABS. Retrieved 30 July 2009, from <www.abs.gov.au/ausstats/[email protected]/cat/4906.0 >.
- Australian Infant Child Adolescent and Family Mental Health Association. (2004). Principals and actions for services and people working with children of parents with mental illness . Adelaide: AICAFMHA.
- Australian Institute of Health and Welfare. (2009). Child protection Australia 2007-08 (Child Welfare Series No. 45). Canberra: AIHW. Retrieved 14 May 2009, from <www.aihw.gov.au/publications/ >.
- Barr, R. G., Trent, R. B., & Cross, J. (2006). Age-related incidence curve of hospitalized Shaken Baby Syndrome cases: Convergent evidence for crying as a trigger to shaking. Child Abuse & Neglect, 30 (1), 7-16.
- Biehal, N. (2007). Reuniting children with their families: Reconsidering the evidence on timing, contact and outcomes. British Journal of Social Work, 37 (5), 807-803.
- Blake, W. (1982) Infant sorrow. In P. Butter (Ed.), William Blake: Selected poems. London: J. M. Dent. (Original work published 1794)
- Blakester, A. (2006). Practical child abuse and neglect prevention. Child Abuse Prevention Newsletter, 14 (2), 2-10.
- Booth, T., & Booth, W. (1993). Parenting with learning difficulties: Lessons for practitioners. British Journal of Social Work, 23 , 459-480.
- Bowlby, J. (1969). Attachment and loss: Vol. 1. Attachment. London: Hogarth Press.
- Bowlby, J. (1980). Attachment and loss: Vol. 3. Loss: Sadness and depression. London: Hogarth Press.
- Bradley, B. S. (1989 ). Visions of infancy. Cambridge: Polity Press.
- Brazelton, T. B., & Cramer, B. G. (1990). The earliest relationship: Parents, infants, and the drama of early attachment. Reading, MA: Addison-Wesley.
- Brisch, K. H. (2004). Treating attachment disorders: From theory to therapy. New York: Guilford Press.
- Bromfield, L. M., Gillingham, P., & Higgins, D. J. (2007). Cumulative harm and chronic child maltreatment. Developing Practice, 19 , 34-42.
- Bromfield, L. M., & Holzer, P. J. (2008). A national approach for child protection: Project report. Melbourne: Australian Institute of Family Studies. Retrieved 14 May 2009, from <www.aifs.gov.au/sites/default/files/nch/pubs/reports/cdsmac/cdsmac.pdf >.
- Bunston, W. (2008). Baby lead the way: Mental health group work for infants, children and mothers affected by family violence. Journal of Family Studies, 14 , 334-341.
- Butchart, A., & Phinney Harvey, A. (2006). Preventing child maltreatment: A guide to taking action and generating evidence . Geneva: World Health Organization and International Society for Prevention of Child Abuse and Neglect.
- Carlson, V., Cicchetti, D., Earls, F., Farrell, M., Macovei, O., & Nystrom, P. (1989). Disorganized/disoriented attachment relationships in maltreated infants. Developmental Psychology, 25 , 525-531.
- Carter, S. L., Osofsky, J. D., & Hann, D. M. (1991). Speaking for the baby: A therapeutic intervention with adolescent mothers and their infants. Infant Mental Health Journal, 12 (4), 291-301.
- Center on the Developing Child at Harvard University (2007). A science-based framework for early childhood policy: Using evidence to improve outcomes in learning behaviour and health for vulnerable children . Cambridge, MA: Center on the Developing Child at Harvard University. Retrieved 14 May 2009, from <www.developingchild.harvard.edu/content/downloads/Policy_Framework.pdf>.
- Centre for Community Child Health. (2008). Towards an early years learning framework (Policy Brief No. 12). Retrieved 14 May 2009, from <www.rch.org.au/emplibrary/ccch/PB12_Towards_EY_Learn_Fwork.pdf >.
- Centre for Community Child Health. (2009). The impact of poverty on early childhood development. Melbourne: Centre for Community Child Health.
- Children's Protection Society. (2007). CPS strategic plan: Early intervention strategy. Intervening early in life. Melbourne: Children's Protection Society.
- Cousins, C. (2005). But the parent is trying ...: The dilemmas workers face when children are at risk from parental substance use. Child Abuse Prevention Newsletter, 13 (1), 3-6.
- Council of Australian Governments. (2009). <Protecting children is everyone's business: National Framework for Protecting Australia's Children 2009-2020> . Canberra: COAG. Retrieved 31 July 2009, from <www.fahcsia.gov.au/our-responsibilities/families-and-children/publications-articles/protecting-children-is-everyones-business>.
- Commission for Children and Young People and Child Guardian. (2008). Child Death Case Review Committee Annual Report 2007-08: Reviews of child deaths known to the Queensland Child Protection System . Brisbane: Commission for Children and Young People and Child Guardian.
- Commission on Social Determinants of Health. (2008). Closing the gap in a generation: Health equity through action on the social determinants of health. Final Report of the Commission on Social Determinants of Health . Geneva, World Health Organization.
- Dawe, S. (2007). Substance use and abuse: An update for child safety officers. Paper presented at the Parental Substance Misuse and Child Protection, Department of Child Safety Research Forum.
- Dawe, S., Harnett, P. H., & Frye, S. (2008). Improving outcomes for children living in families with parental substance misuse: What we know and what should we do (Child Abuse Prevention Issues No. 29). Melbourne: Australian Institute of Family Studies. Retrieved 14 May 2009, from <www.aifs.gov.au/nch/pubs/issues/issues29/issues29.html>.
- DeBellis, M. (2001). Developmental traumatology: The psychobiological development of maltreated children and its implications for research, treatment and policy. Development and Psychopathology, 13 , 539-564.
- DePanfilis, D., & Zuravin, S. J. (1999). Predicting child maltreatment recurrences during treatment. Child Abuse and Neglect, 23 (8), 729-743.
- Department of Health and Ageing. (2008). Improving maternity services in Australia: A discussion paper from the Australian Government. Canberra: Department of Health and Ageing.
- Department of Health and Community Services. (2007). Recommendations of a review conducted in relation to the deaths of a number of children involved with the child protection system in Tasmania. Hobart: Department of Health and Human Services. Retrieved 7 August 2009, from <www.dhhs.tas.gov.au/__data/assets/pdf_file/0005/36716/Recommendations_from_ChildDeath_Review2007.pdf>
- Dice, J. L., Claussen, A. H., Katz, L. F., & Cohen, J. B. (2004). Parenting in Dependency Drug Court. Juvenile and Family Court Journal, 55 (3), 1-10.
- Dowdney, L., & Skuse, D. (1993). Parenting provided by adults with mental retardation. Journal of Child Psychology and Psychiatry, 34 (1), 25-47.
- Dozier, M., & Lindhiem, O. (2006). This is my child: Differences among foster parents in commitment to their young children. Child Maltreatment, 11 (4), 338-345.
- Drell, M., Siegel, C., & Gaensbauer, T. (1993). Post traumatic stress disorder. In C. Zeanah (Ed.), Handbook of infant mental health (pp. 291-304). New York: Guildford Press.
- Edwards, B., Wise, S., Gray, M., Hayes, A., Katz, I., Misson, S. et al. (2009). Stronger Families in Australia study: The impact of Communities for Children (Occasional Paper No. 25). Canberra: Department of Families, Housing, Community Services and Indigenous Affairs. Retrieved 31 July 2009, from <www.fahcsia.gov.au/our-responsibilities/families-and-children/publications-articles/number-25-stronger-families-in-australia-study-the-impact-of-communities-for-children>.
- Families Australia. (2007). Towards a national child protection strategy for Australia. Canberra: Families Australia. Retrieved 14 May 2009, from <www.familiesaustralia.org.au/publications/pubs/cpsdraft.pdf >.
- Fegran, L., Helseth, S., & Fagermoen, M. S. (2008). A comparison of mothers' and fathers' experiences of the attachment process in a neonatal intensive care unit. Journal of Clinical Nursing, 17 , 810-816.
- Feldman, M. (2004). Self-directed learning of child care skills by parents with intellectual disabilities. Infants and Young Children, 17 (1), 17-31.
- Feldman, M., & Léger, M. (1997). Stress in mothers with intellectual disabilities. Journal of Child and Family Studies, 6 (4), 471-485.
- Fonagy, P. (1998). Prevention: The appropriate target of infant psychotherapy. Infant Mental Health Journal, 19 (2), 121-150.
- Fraiberg, S., & Shapiro, V. (1980). Clinical studies in infant mental health: The first year of life. London: Tavistock Publications.
- Frame, L., Berrick, J., & Coakley, J. (2006). Essential elements of implementing a system of concurrent planning. Child & Family Social Work, 11 (4), 357-367.
- Gauthier, Y., Fortin, G., & Je Liu, G. (2004). Clinical application of attachment theory in permanency planning for children in foster care: The importance of continuity of care. Infant Mental Health Journal, 25 (4), 379-396.
- Gilberg, C., & Geiger-Karlsson, M. (1993). Children born to mentally retarded women: A 1-21 year follow up study of 41 cases. Psychological Medicine, 13 , 891-894.
- Goldfeld, S. R., Wright, M., & Oberklaid, F. (2003). Parents, infants and health care: Utilization of health services in the first 12 months of life. Journal of Paediatrics and Child Health, 39 , 249-253.
- Goldsmith, D. F., Oppenheim, D., & Wanlass, J. (2004). Separation and reunification: Using attachment theory and research to inform decisions affecting the placements of children in foster care. Juvenile and Family Court Journal, 55 (2), 1-14.
- Harris, N. (2008). Family group conferencing in Australia: Ten years on (Child Abuse Prevention Issues No. 27). Melbourne: Australian Institute of Family Studies.
- Higgins, D., & Katz, I. (2008). Enhancing service systems for protecting children: Promoting child wellbeing and child protection reform in Australia. Family Matters, 80 , 43-50.
- Hill, S. L., & Solchany, J. (2005). Mental health assessments for infants and toddlers (Child Law Practice Vol. 24, No. 9). Washington, DC: Zero to Three.
- Householder, J., Hatcher, R., Burns, W., & Chasnoff, I. (1982). Infants born to narcotic-addicted mothers. Psychological Bulletin, 92 (2), 453-468.
- Humphreys, C. (2007). Talking to my mum: Strengthening relationships between mothers and children in the aftermath of family violence. Developing Practice: The Child, Youth and Family Work Journal, 19 , 12-15.
- Humphreys, C., Houghton, C., & Ellis, J. (2008). Literature review: Better outcomes for children and young people experiencing domestic abuse . Edinburgh: Scottish Executive Domestic Abuse Delivery Group. Scottish Government. Retrieved 30 July 2009, from <www.scotland.gov.uk/Publications/2008/08/04112614/0 >.
- Humphreys, C., & Kiraly, M. (2009). Baby on board: Report of the Infants in Care and Family Contact Research Project . Melbourne: Alfred Felton Research Program, School of Nursing and Social Work, University of Melbourne.
- Klein, R., Gilkerson, L., & Davis, E. (2008). Prenatal development. Washington, DC: Zero to Three. Retrieved 31 July 2009, from <www.zerotothree.org/site/DocServer/EarlyBrain_Unit2.pdf?docID=4461 >.
- Larrieu, J. A., Heller, S. S., Smyke, A. T., & Zeanah, C. H. (2004). Predictors of permanent loss of custody for mothers of infants and toddlers in foster care. Infant Mental Health Journal, 29 , 48-60.
- Leckman, J., & Mayes, L. (2007). Nurturing resilient children. Journal of Child Psychology and Psychiatry, 48 (3-4), 221-223.
- Lieberman, A. F. (2004). Traumatic stress and quality of attachment: Reality and internalization in disorders of infant mental health. Infant Mental Health Journal, 25 (4), 336-351.
- Lieberman, A. F., Van Horn, P., & Gosh Ippen, C. (2005). Toward evidence-based treatment: Child parent psychotherapy with preschoolers exposed to marital violence. Journal of American Academy of Child and Adolescent Psychiatry, 44 (12), 1241-1248.
- Llewellyn, G., & McConnell, D. (1998). Perception of service needs by parents with intellectual disability, their significant others and their service workers. Child Abuse Neglect, 19 (3), 245-260.
- Llewellyn, G., & McConnell, D. (2003). Prevalence and outcomes for parents with disabilities and their children in an Australian court sample. Child Abuse and Neglect, 27 (3), 233-251.
- MacMillan, H. L., Wathen, C. N., Barlow, J., Fergusson, D. M., Leventhal, J. M., & Taussig, H. N. (2009). Interventions to prevent child maltreatment and associated impairment. Lancet, 373 , 250-266.
- Mbwili-Muleya, C., Gunn, J., & Jenkins, M. (2000). General practitioners: Their contact with maternal and child health nurses in postnatal care. Journal of Paediatrics & Child Health, 36 , 159-163.
- McHugh, M. (2003, 12-14 February 2003). Paying for care: The state of affairs in fostering. Paper presented at the 8th Australian Institute of Family Studies Conference, Melbourne.
- Melmed, M. E. (2004). Statement of Matthew E. Melmed, Executive Director, Zero to Three: National Center for Infants, Toddlers and Families. Before the House Committee on Ways and Means Subcommittee on Human Resources, June 17 2004 .
- Meltzoff, A. N., & Brooks, R. (2007). Intersubjectivity before language: Three windows on preverbal sharing. In S. Bråten (Ed.), On being moved: From mirror neurons to empathy (pp. 149-174). Philadelphia, PA: John Benjamins.
- Mrazek, P. J. (1993). Maltreatment and infant development. In C. H. Zeanah (Ed.), Handbook of infant mental health (pp. 159-170). New York: Guildford Press.
- Murray, L. (2006). Intersubjectivity, object relations theory, and empirical evidence from mother-infant interactions. Infant Mental Health Journal, 12 (3), 219-232.
- National Clearinghouse on Child Abuse and Neglect Information, & National Adoption Information Clearinghouse. (2005). Concurrent planning: What the evidence shows. Washington, DC: National Clearinghouse on Child Abuse and Neglect Information and National Adoption Information Clearinghouse.
- National Institute of Child Health and Human Development Early Child Care Research Network. (2003). Does amount of time spent in child care predict socioemotional adjustment during the transition to kindergarten? Child Development, 74 (4), 976-1005.
- Newman, L., & Stevenson, C., (2005). Parenting and borderline personality disorder: Ghosts in the nursery. Clinical Child Psychiatry and Psychology, 10 (3), 385-394.
- Nielssen, O. B., Large, M. M., Westmore, B. D., Lackersteen, S. M. (2009). Child homicide in New South Wales from 1991-2005. Medical Journal of Australia, 190 (1), 7-11.
- Nylen, K. J., Moran, T. E., Franklin, C. L., & O'Hara, M. W. (2006). Maternal depression: A review of relevant treatment approaches for mothers and infants. Infant Mental Health Journal, 27 (4), 327-343.
- O'Donnell, M., Scott, D., & Stanley, F. (2008). Child abuse and neglect: Is it time for a public health approach? Australian and New Zealand Journal of Public Health, i(4), 325-330.
- Olds, D. (2006). The nurse-family partnership: An evidence based preventative intervention. Infant Mental Health Journal, 27 (1), 5-25.
- Osofsky, J. D., Hann, D. M., & Peebles, C. (1993). Adolescent parenthood: Risks and opportunities for parents and infants. In C. H. Zeanah (Ed.), Handbook of infant mental health (pp. 106-119). New York: Guildford Press.
- Parslow, R. C., Tasker, R. C., Draper, E. S., Parry, G. J., Jones, S., Chater, T., et al. (2009). Epidemiology of critically ill children in England and Wales: Incidence, mortality, deprivation and ethnicity. Archives of Disease in Childhood, 94 , 210-215.
- Perry, B. D. (2002). Childhood experience and the expression of genetic potential: What childhood neglect tells us about nature and nurture. Brain and Mind, 3 (1), 79-100.
- Poobalan, A. S., Aucott, L. S., Ross, L., Smith, W. C., Helms, P. J., & Williams, J. H. (2007). Effects of treating postnatal depression on mother-infant interaction and child development: Systematic. British Journal of Psychiatry, 191 , 378-386.
- Quinlivan, J. A., Peterson, R. W., & Gurrin, L. C. (1999). Adolescent pregnancy: Psychopathology missed. Australian and New Zealand Journal of Psychiatry, 33 , 864-868.
- Reading, R., Bissel, S., Goldhagen, J., Harwin J., Masson J., Moynihan S. et al. (2008). Promotion of children's rights and prevention of child maltreatment. The Lancet, 373 (9660), 332-343.
- Reebye, P. N., Ross, S. E., & Jamieson, K. (2008). A literature review of child-parent/caregiver attachment theory and cross cultural practices influencing attachment . Toronto: St. Joseph's Women's Health Centre. Retrieved 14 May 2009, from <www.attachmentacrosscultures.org/research>.
- Richardson, N., Irenyi, M., Kelleher, J., & Horsfall, B. (2009). Children in care (Resource Sheet No. 8). Melbourne: Australian Institute of Family Studies. Retrieved 14 May 2009, from <www.aifs.gov.au/nch/pubs/sheets/rs8/index.html>.
- Royal Australian College of Physicians. (2006). Health of children in "out-of-home" care. Sydney: RACP. Retrieved 14 May 2009, from <www.racp.edu.au/download.cfm?DownloadFile=A8C23B50-2A57-5487-D72BB868F7C9BF16 >.
- Schmeid, V., Homer, C., Kemp, L., Thomas, C., Fowler, C., & Kruske, S. (2008). The role and nature of universal health services for pregnant women, children and families in Australia . Canberra: Australian Research Alliance for Childhood and Early Years. Retrieved 14 May 2009, from <www.aracy.org.au/publicationDocuments/TOP_The_role_and_nature_of_universal_health_services_for_pregnant_women_children_and_families_in_Australia_2008.pdf>.
- Scott, D. (2006). Towards a public health model of child protection in Australia. Communities, Children and Families Australia, 1 , 9-16.
- Seabrook, J. (2008, 10 November). Suffering souls: The search for the roots of psychopathy. The New Yorker. Retrieved 14 May 2009, from <www.newyorker.com/reporting/2008/11/10/081110fa_fact_seabrook >.
- Seifer, R., & Dickstein, S. (1993). Parental mental illness and infant development. In C. H. Zeanah. (Ed.), Handbook of infant mental health (pp. 145-160). New York: Guildford Press.
- Seligman, S. (1994). Applying psychoanalysis in an unconventional context: Adapting parent psychology to a changing population. Psychoanalytic Study of the Child, 49 , 481-500.
- Shonkoff, J. P., & Phillips, D. A. (Eds.). (2001). From neurons to neighbourhoods: The science of early childhood development (2nd Ed.). Washington, DC: National Academy Press.
- Siegel, D. (2001). Toward an interpersonal neurobiology of the developing mind: Attachment relationships, mindsight and neural integration. Infant Mental Health Journal, 22 (1-2), 67-94.
- Smariga, M. (2007). Visitation with infants and toddlers in foster care: What judges and attorneys need to know . Washington, DC: Zero to Three.
- Smarsh Hogan, T. M., Myers, B. J., & Elswick, R. K., Child abuse potential among mothers of substance-exposed and nonexposed infants and toddlers. Child Abuse and Neglect, 30 (2), 145-156.
- Stern, D. (2008). The clinical relevance of infancy: A progress report. Infant Mental Health Journal, 29 (3), 177-188.
- Stevenson, O. (2007). Neglected children and their families. Oxford: Blackwell.
- Sved Williams, A. (2004). Infants of mothers with mental illness. In V. Cowling (Ed.), Children of parents with mental illness (pp. 17-40). Melbourne: ACER.
- Taft, A., Watson, L., & Lee, C. (2004). Violence against young Australian women and association with reproductive events: A cross-sectional analysis of a national population sample. Australian and New Zealand Journal of Public Health, 28 (4), 324-9.
- United Nations. (1989). Convention on the Rights of the Child. Geneva: Office of the High Commissioner for Human Rights. Retrieved April 2009, from <www.unhchr.ch/html/menu3/b/k2crc.htm>.
- Victorian Child Death Review Committee. (2008). Annual report of inquiries into the deaths of children known to Child Protection 2008 . Melbourne: Victorian Child Death Review Committee. Retrieved 28 November 2008, from <www.ocsc.vic.gov.au/downloads/vcdrc/ar_web.pdf>.
- Walker, P., & Youcha, V. (2006). Forming healthy attachments for our most vulnerable population. Paper presented at the 12th Annual Drug Court Training Conference.
- Wilensky, S., & Prosser, M. (2008). Community approaches to women's health: Delivering preconception care in a community health centre model. Women's Health Issues, 18 (6), S52-S60.
- Wood, J. (2008). Report of the Special Commission of Inquiry into Child Protection Services in NSW: Executive summary and recommendations . Sydney: Department of Premier and Cabinet. Retrieved 14 May 2009 from <www.dpc.nsw.gov.au/publications/news/stories/?a=33794>.
- Wright, C. M., Jeffrey, S. K., Ross, M. K., Wallis, L., & Wood, R. (2009). Targeting health visitor care: Lessons from Starting Well. Archives of Disease in Childhood, 94 , 23-27.
- Yeo, S. S. (2003). Bonding and attachment of Australian Aboriginal children. Child Abuse Review, 12 , 292-304.
- Zeanah, C., & Sheeringa, M. D. (1996). Evaluation of post traumatic symptomatology in infants and young children exposed to violence. Zero to Three, 16 (5), 9-14.
- Zero to Three. (2002). What is infant mental health? Washington, DC: Zero to Three.
- Zero to Three. (2004). Research summary: Children exposed to violence. Washington DC: Zero to Three.
- Zero to Three. (2005). Diagnostic classification of mental health and developmental disorders of infancy and early childhood (Rev. Ed.) (DC 0-3R). Washington DC: Zero to Three.
- Zero to Three. (2006). Court Teams for Maltreated Infants and Toddlers Project: Impact statement. Washington DC: Zero to Three.
- Zuckerman, B., & Brown, E. R. (1993). Maternal substance abuse and infant development. In C. H. Zeanah. (Ed.), Handbook of infant mental health. New York: Guildford Press.
Associate Professor Brigid Jordan has over 20 years' experience as a social worker in child psychiatry and the infant mental health program at the Royal Children's Hospital in Melbourne and is now the Associate Professor Paediatric Social Work (Infant and Family) at the Royal Children's Hospital and the Department of Paediatrics, The University of Melbourne. This position is funded by Melbourne Community Foundation. Associate Professor Jordan heads the Social and Mental Health Aspects of Serious Illness Research Group at the Murdoch Childrens Research Institute.
Robyn Sketchley is a social worker with 9 years' experience in child protection, family support, child psychiatry and infant mental health and currently works in the Royal Children's Hospital Mental Health Service Peek-a-Boo program for infants and their mothers exposed to family violence and at the Murdoch Childrens Research Institute.
The authors gratefully acknowledge the input and assistance provided by Dr Leah Bromfield and the feedback received from peer reviewers. This Issues paper builds upon earlier work conducted by the authors as part of the Specialist Practice Guides project funded by the Victorian Government Department of Human Services and undertaken by the Australian Institute of Family Studies.
In this paper, Brigid Jordan and Robyn Sketchley draw on research and their own extensive experience as practitioners in infant mental health to explore whether a public health approach together with a human rights perspective can provide a framework for service provision that better protects infants from experiencing the damaging effects of abuse and neglect.
1 921414 05 3