Characteristics of carers in Victoria
You are in an archived section of the AIFS website
May 1993
Abstract
The increasing rates of disability and a major shift from custodial to community care for people with severe and chronic disabilities has led to an increasing reliance on families and other unpaid caregivers in the home. How are these carers coping, and what is the impact of caregiving on the health and wellbeing of family carers over time? In this edited version of a paper presented at the fourth Australian Family Research Conference in February 1993, the authors report on the first stage of a major research and intervention program focusing on the wellbeing of families caring for people with a range of severe and long-term illnesses and disabilities. Using a cross-diagnostic approach, the program is using a stress and coping theoretical framework to explore the impact of caregiving on carers over time, the variety of responses to this role and use of services.
Relatives and other unpaid caregivers in the home are major sources of support for people with long-term illness and severe disabilities. With an ageing population, increasing rates of disability and the growth in 'community care', the role of the family caregiver has expanded in recent years and will continue to expand. (McCallum 1992a, 1992b; Otis and Howe 1991; Rosenman 1991)
It is not surprising, therefore, that family caregiving is becoming a major focus of research interest overseas (Green 1985; Hooyman 1990; Levin et al 1989; and more recently in Australia (Braithwaite 1990; Brodaty and Gresham 1989; Draper et al 1992; Draper et al 1992; Schultz and Schultz 1990). Moreover, in recent years informal carers have been gaining some recognition in government policy at the state and federal levels (Bozic (in press); Mid-Term Review 1991).
Even so, there is little local information about the prevalence of caregiving and the socio-demographic characteristics of caregivers. In Australia, the most reliable information comes from the Australian Bureau of Statistics' 1988 Survey of Disabled and Aged Persons which included questions related to co-resident caregivers.
Furthermore, there is little local information on the impact of caregiving on the physical and emotional wellbeing of the caregiver. Research to date, largely overseas, suggests that the levels of stress involved in caregiving can be high and may result in psychiatric disturbance in the caregivers themselves (Morris et al1988.)
To date, research has largely focused on carers in particular disability groups (for example, dementia, schizophrenia, intellectual disability) and, for the most part, has been based on small samples drawn from support organisations or service providers. Family caregiving covers the full spectrum of ages and life stages, illnesses and disabilities. Caregivers can be mothers, daughters, sons, spouses, close friends or neighbours. Sampling and methodological limitations have not permitted the exploration of differences between these groups. Moreover, most studies have been cross-sectional. See Herrman, Singh, Schofield, Eastwood, Burgess, Lewis and Scotton (in press) for an overview of overseas and local research, Raveis, Siegel and Sudit (1988-89) for a critical review of past research, Braithwaite (1992), Murphy, Schofield and Herrman (1992) and Pearlin et al (1990) for analyses of relevant conceptual and measurement issues.
Overall, it is unclear which generic factors, including service provision, are important in influencing the experience of caregiving. We do not know the significance of factors specific to groups defined either by disability or age of the care recipient, or by age, sex, socio-economic status or other characteristics of the caregiver.
THE CARERS' PROGRAM
The Victorian Health Promotion Foundation is supporting a major research and intervention program focusing on the wellbeing of families caring for people with a range of severe and long-term illnesses and disabilities.
Employing a cross-diagnostic approach, the program is using a stress and coping theoretical framework to explore the impact of caregiving on carers over time, the variety of responses to this role and use of services. Findings from the longitudinal research study and from a review of health promotion activities will be used to identify intervention strategies to assist carers in their caregiving role. The two aspects of the program (research and interventions) will proceed in parallel and interact with each other. That is to say, information progressively available from the research study will be used in the design of interventions. The implementation and evaluation of interventions in specific groups will be incorporated within the longitudinal research study on the effects of caregiving.
More specifically, the study aims to survey the distribution of informal caregiving in Victoria, assess the impact of caregiving on the emotional and physical wellbeing of family carers, explore the experience of caregiving, the problems and the supports, and identify services and strategies used by caregivers which help to ease their burden.
This paper reports some preliminary findings from the first wave of data collection in the first stage of the study. Because of the breadth and complexity of the study, involving as it does the full spectrum of family caregivers, and in order to obtain an accurate profile of carers in the state, we estimated that we would need a representative sample of approximately 1000 caregivers. We further estimated that one or more caregivers would be identified in between 5 and 10 per cent of households surveyed, and that a proportion of those would decline to be interviewed. In order to allow a more accurate calculation of the number of households to be surveyed and a meaningful assessment of the effectiveness of our method, screening questions and interview, it was decided to start with an initial survey of 2000 households.
A questionnaire was developed to identify and obtain information from carers of people with disabilities and a comparison group of 'non-carers'. Information was sought in relation to socio-demographic characteristics, aspects of the caring role including social and emotional responses, service use, measures of social support, coping strategies, health and emotional wellbeing of the carer, life satisfaction and so on.
Using the Australian Institute of Family Studies' computer assisted telephone interviewing (CATI) system and a team of trained interviewers, a statewide random survey of 2000 telephone numbers was conducted in November 1992.
Excluding 305 telephone numbers which were found to be disconnected, non-residential or non-contactable (engaged or not answered on repeated occasions), 91 per cent of contacted households were screened: that is, 9 per cent refused to answer screening questions. Of the 136 caregivers identified, 72 per cent agreed to be interviewed. The response rate for the comparison group was a slightly lower 68 per cent. The proportion of households in which a carer was identified was calculated at 9 per cent.
FINDINGS
The CATI system was found to be an effective method of gathering data from family caregivers in that it was relatively non-intrusive and allowed the flexibility of both precoded and free response questions. Most importantly, the fact that 98 per cent of carers agreed to be interviewed on subsequent occasions suggests that they felt comfortable with the method and content of the interview.
Here, presentation of findings is limited to descriptive information about the sample of carers, and no comparisons are made with the sample of 'non-carers'. What the findings reflected most was the heterogeneity of carers and the diversity of caregiving roles and circumstances.
CHARACTERISTICS OF CAREGIVERS
As shown in Table 1, there were both men and women carers, but not surprisingly women predominated (79 per cent). Caregivers covered a large spectrum of ages from 15 to 80 but, consistent with other research, most fell in the middle age ranges, with more than 70 per cent aged between 30 to 59 years of age. Most (over three quarters) were married.

There was diversity, too, in terms of the carer's relationship to the care recipient (Table 2). The largest group comprised adult children (41 per cent), mostly daughters, caring for parents. Next came parents (26 per cent), again mostly mothers, caring for children. Then came those caring for a spouse or partner (19 per cent), of whom most were wives caring for their husbands. The remaining 14 per cent were caring for a range of other relatives including parents-in- law, grandparents and siblings, and a tiny handful caring for friends.

Living arrangements were another source of variation. A little over half the caregivers (54 per cent) lived with the person they were caring for. A relatively high 22 per cent of care recipients lived alone, and 15 per cent lived in residential care (Table 3).

All spouse caregivers and the vast majority (84 per cent) of parents caring for their children were co-resident. Conversely, daughters and sons (43 per cent) were likely to be caring for a parent who lived alone: 25 per cent of parents received live-in care from their children and an equivalent proportion were in residential care.
The length of time carers had been providing care for their relatives ranged from one month to 27 years. Most participants, in fact, had been caring for their relatives for some years, and for a sizeable minority it was in excess of five, even ten years (Table 4).

As Table 5 shows, the amount of time carers spent caring for relatives varied from 7 days a week for 57 per cent of the sample to one day or less for 19 per cent. Marked variations were associated with living arrangements.

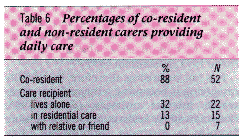
As Table 6 shows, for most co-resident carers (88 per cent), their caring role was seven days a week. For non- resident carers the time spent caring varied depending on where their relative was living. Understandably, carers were more likely to provide daily support to family members who lived alone than to relatives living in residential care or with another relative or friend. That is, 32 per cent of carers of people living alone provided daily assistance compared with 13 per cent of the small number whose relatives were in residential care, and none of the carers of family members living with other relatives or friends.
CARE RECIPIENT CHARACTERISTICS
A little over half the care recipients were female (Table 7). Consistent with the greater longevity of women, daughters and sons for the most part were caring for their mothers with only a small proportion caring for fathers. However, when it came to parents caring for children, there were more sons than daughters with illness or disability: again, this is consistent with differential rates of disability between boys and girls.
Table 7 also shows that care recipients ranged in age from four to 98 years of age. However, whereas there was a concentration of caregivers in the middle age ranges, the converse was true for care recipients. Care recipients were predominantly in the older age groups with almost half being 75 years or more and, to a lesser extent, in the young: 17 per cent were children under 14 years of age.

ILLNESS OR DISABILITY
Regarding long-term illness or disabling condition: around 90 per cent of care recipients had multiple problems. Responses to open-ended questions indicated a wide range of conditions including multiple age-related problems, diabetes, stroke, dementia, heart disease, cancer, arthritis, asthma, musculoskeletal problems including limb amputation, psychiatric problems, developmental delay and so on.
Carers were asked, in lay terminology, with examples, whether their relatives suffered from any of the broadly categorised disabilities (listed in Table 8) and, if so, whether the problem was mild, moderate or severe. Almost half were reported as having moderate or severe physical/mobility problems, and in the majority of cases the problem was severe. Similar proportions also had problems with fine motor coordination. Not surprisingly, those with mobility problems also tended to have coordination problems. Mobility problems were significantly associated with increasing age.

Around 40 per cent had long-term health problems which in some cases constituted the major illness or disabling condition. With sensory loss, it was only in a handful of cases that hearing or visual impairment was specified as the main disabling condition. However, with increasing age came increasing proportions of care recipients with sensory loss - 70 per cent in the case of those over 65 years of age.
About a third of the care recipients had psychiatric or emotional problems of a severe or moderate kind. Similar proportions were impaired intellectually. Those with intellectual problems tended to have emotional problems and difficulties in communication, such as speech difficulties or in understanding others.
Overall, 56 per cent of care recipients were reported as having at least one severe disability, 36 per cent with at least one moderate disability and a low 6 per cent with mild impairments only. A little over half used special aids or equipment such as walking frames or hearing aids.
CARING ROLE
A common feature of caregiver research is obtaining information about assistance with activities of daily living. In the present study such information was not sought from parents of children with disabilities under the age of six years (N = 6) on the assumption that assistance would be provided even in the absence of impairment. Help needed and given, of course, will vary with the impairments of the care recipient and the capacities and inclination of the care giver.
According to carers (Table 9), the tasks for which assistance was most frequently needed were organising appointments and social services (63 per cent) and going out (61 per cent). About half needed help with managing money, such as keeping track of expenses and paying bills (52 per cent). A little over a third needed assistance with personal care tasks such as bathing, showering (36 per cent) and dressing (35 per cent). A relatively high 26 per cent needed assistance with incontinence problems and a similar proportion with getting in and out of bed. Non- resident carers were also asked about assistance with general household tasks: help with shopping (82 per cent), repairs around the house (81 per cent) and general housework (77 per cent) were those most often needed.

There was a clustering in carers' activities. Not surprisingly, carers who helped their relatives to bathe or shower were also more likely to help with dressing, using the toilet, incontinence problems and getting in and out of bed or a chair. Help needed with the latter, implying limited mobility, was also linked with various other mobility-related tasks including using the toilet, dressing and moving about the house. Similarly, carers who organised their relatives' appointments and social services were also likely to be managing their money. For non-resident carers, those who helped with washing also assisted with cooking and general housework.
As shown in Table 10, in addition to the special assistance given to relatives because of their illness or disability, most of the caregivers had the main responsibility for the day- to-day tasks for the whole household. That is, 75 per cent cooked, washed and ironed for their families, and around 70 per cent undertook the light and heavy household chores including vacuuming and cleaning the bathroom, shopped and organised health and social services. Moreover, more than half the carers (57 per cent) said that they spent extra time doing these chores because of their caregiving responsibilities.

BEHAVIOUR PROBLEMS
Caring for a relative with a chronic illness or disability often involves dealing with difficult behaviours. Carers reported that the most common forms of difficult behaviour were the repetition of questions and stories, the inability to concentrate, being cranky or easily irritated, listless and fatigued, forgetful or confused. Between 60 to 70 per cent of carers said their relatives 'often' or 'sometimes' behaved in these ways (Table 11).

Behaviour problems often clustered together. For example, those who were easily irritated were more likely to have very changeable moods, be uncooperative, aggressive even suspicious or accusing. Forgetfulness and confusion were linked with an inability to concentrate, being withdrawn, hardly ever speaking and being fearful and afraid.
Most carers (77 per cent) indicated that their relatives had at least one behaviour problem 'often' exhibited. Moreover, a relatively high 39 per cent of carers found their relatives' behaviour problems difficult or very difficult to cope with.
Carers were asked to comment on the most difficult aspects of their relatives' behaviour. While some talked about the emotional and physical pressures of dealing with particular behaviour problems, others talked of their long- term anxieties about their relatives, the effect of the disabling condition on their lives, the imminent mortality of a loved one, the loss of companionship of the person they used to know.
A young mother caring for her six-year-old son with asthma and communication problems said: 'His tantrums, they just go on and on, yelling, screaming .... he just stiffens and I can't lift him.' Another mother had similar problems with her 11-year- old with intellectual impairment: 'I can't cope with his frustration ... he beats his chest and bites his fingers.'
In contrast, is a mother whose seven-year-old son has a physiological condition resulting in incontinence: 'that it is most likely for life and how that will affect him,' was the most upsetting aspect. Likewise, a mother caring for her young adult son with HIV: in spite of severe behavioural and emotional problems, 'the fact that he will die soon,' was the most difficult aspect to come to terms with.
For a father caring for his 17-year-old son with some intellectual impairment and psychiatric problems, 'trying to get him active ... to keep him occupied,' was the most difficult thing: 'Thoughts go through his head, he just sits there and cries - it could happen ten times a day.'
'I hate seeing her sad,' was the response of a schoolgirl caring for her mother with a disabling and terminal illness; while for a 35-year-old daughter caring for her mother with Alzheimers' disease it was 'the fact that she's aggressive and doesn't know who I am'; and for a 78-year-old wife caring for her husband aged 79 with Parkinsons Disease it was 'not having him with me when I go out.'
USE OF COMMUNITY SERVICES
Considering the shift away from institutional care in favour of home-based or community care, the use of formal services to assist in family caregiving is of particular interest in the current program. However, excluding those whose relatives were in residential care, only a minority of the respondents received regular formal services to assist in their caring role (Table 12a). Transportation (for example, multi-purpose taxis or community buses) and general home help were the most frequently used services but, even so, only by 17 per cent of carers. Specific home help (that is, assistance with minding, bathing, caring for their relative) was used by 12 per cent of carers with a similar proportion using a community nursing service. The Meals on Wheels service was received by 7 per cent.
It is perhaps relevant that less than half the carers (47 per cent) had received any information about relevant services and organisations. Comments regarding services included: 'There must be services out there that we need but do not know are out there.' 'I haven't sought anything so I don't know what's available.'

In the case of one-time services (Table 12b), 29 per cent had received home modifications (for example, ramps, handles, rails) to assist caring for their relatives. Counselling or therapy related to their relative's condition had been received by 18 per cent of carers, and a handful had done a training course to learn skills related to their caring role. While only 5 per cent of the carers had had any kind of respite care for their relatives in the past 12 months, 20 per cent said they would like it. However, the most common reason for not using respite care was that they didn't need it (59 per cent) or that their relative wouldn't like it (15 per cent). Some had not heard of it. Other carers expressed reluctance: 'I'd rather have her go somewhere she knows the person,' was one comment; 'I'd rather look after her myself ... it's my responsibility,' was another.
Although most respondents expressed satisfaction with each service used, the low numbers receiving services preclude interpretation.
Membership of support organisations was low (12 per cent). This is particularly interesting in that much past research has been based on samples drawn from support organisations.
MEDICAL AND HEALTH SERVICES
In contrast to the use of general services, most care recipients had seen a medical or health practitioner in the past six months for problems or tests related to their condition (Table 13). As general practitioners are usually the first contact with health services, it is not surprising that a very high 89 per cent of care recipients had seen their general practitioners in the past six months. Most carers (75 per cent) expressed satisfaction with the service received. While few care recipients had visited a psychologist or psychiatrist (11 per cent), around half had seen other medical specialists (for example, orthopaedic surgeon, paediatrician, geneticist) and other health specialists such as audiologists, social workers). Positive appreciation for the professional attention was commonly expressed.

Considering the high proportion with age-related disabilities, it is perhaps surprising that only 18 care recipients overall (and 26 per cent of those 65 years or over) had been assessed by a geriatric assessment team. A relatively high 43 per cent of care recipients had spent nights as a patient in a hospital which, in most cases, was in the public system.
Concerning information, advice and communication: 77 per cent of carers were generally satisfied with the level of communication between the various medical and health professionals looking after their relative. Likewise, most (74 per cent) were comfortable with the information that they had received about their relatives' condition.
INFORMAL SUPPORT
Although few carers received help in caring for their relative from local services, over half (58 per cent) were supported by family and friends. Help came from siblings, parents, children, partners, other relatives and friends. However, this was mainly in the form of friendship, emotional support and visiting, with very few receiving help in the form of shopping, housework, respite care, nursing/personal care or child minding. Even so, there was positive appreciation expressed by all but six of the carers who were supported in this way. Only 36 per cent of carers overall wanted more help from family and friends. Again, what was most needed was friendship/moral support and visiting, as well as more practical assistance with household chores.
Carers commented about the good and bad aspects of family and friends helping. Despite the severity of his disabilities, one 67-year-old mother who has been caring for her 43-year-old son since the age of 17 when he suffered traumatic brain damage, emphasised the positive aspects of caregiving. Not only did she herself find 'none of his behaviours too difficult to cope with', she also noted that the good thing about family and friends helping in caring for her son is that 'they love him'. Theirs is a 'close family, and caregiving makes us closer, in a way'.
A wife aged 32 caring for her husband aged 42, also with traumatic brain damage noted in relation to support from family and friends: 'It takes the strain off me and they gain an understanding of the difficulties I'm having ... but it's inconvenient for them, it places a burden on them which is not their responsibility ... it also puts [care recipient] into a situation he'd rather not be ... I feel guilty because I have to ask them ... I don't want to put them out.'
For some carers, tension between family members was created through differences in opinions regarding caring responsibilities and difficulty accepting the relative's disability. 'He was really sick and I got accused of not looking after him ... that caused a big blue,' commented a daughter caring for elderly and severely disabled father. 'My brother causes trouble because he can't accept Mum's disability,' were the feelings expressed by another daughter, in this case caring for her mother with Alzheimer's disease.
Assistance from her family and friends had not been sought by one mother caring for her son with psychiatric and drug use problems: 'They'd have a pink fit if they found out ... they're intolerant to drug use and the reasons for drug use ... their overall ignorance wouldn't help a bit.'
CARER HEALTH
Briefly, 42 per cent of carers indicated that they had experienced major health problems in the past year, and a third reported having a long-term illness or disability themselves. Furthermore, almost two thirds agreed that they were exhausted when they went to bed at night and around half felt that they had more things to do than they could handle. The proportions of carers experiencing health and overload problems seem high. However, before any inferences can be drawn about the possible relationship between health problems and caregiving, analyses contrasting our carer sample with our comparison group need to be undertaken. The same is true for our measures of carer wellbeing. Findings in relation to the health of caregivers underline the importance of having a comparison group of people who are not caring for someone with special needs.
EMPLOYMENT AND FINANCIAL CONSIDERATIONS
For some carers the effects of their caregiving role on employment opportunities have obvious financial implications. As Table 14 shows, a little over half the carer sample was not in paid employment. Mostly these carers were engaged in home duties or retired, a small number were full-time students or were unemployed and looking for work. While only 8 per cent of those not in paid employment indicated that they had had to give up their jobs, 20 per cent felt unable to take a job because of their caring commitments.

Although work was a source of relief and an opportunity to develop other interests for over half those in paid employment, it was also a source of competing demands: a majority worried about their relatives while at work and some complained of repeated interruptions during working hours. Not insubstantial numbers indicated that their caregiving responsibilities meant they had less energy for work (28 per cent), had had to take periods of unpaid leave (28 per cent) and work fewer hours (20 per cent). Caregiving for some had meant refusing promotion or taking a less responsible job.
A mother in her thirties caring for a son with cerebral palsy commented, 'Not being able to go to work has a big change on finances.' Similarly, a woman in her early forties caring for her husband with kidney failure and related problems, said, 'There's no real avenue in this situation for someone to keep their job.' Another mother caring for her young adult son with psychiatric and drug-related problems noted other costs in caregiving, besides the emotional ones, as, 'legal fees, doctors, and keeping him out of jail.'
SUMMARY AND CONCLUSION
Many studies in the past have used stringent criteria to define a caregiver - time spent caring, number of activities of daily living for which help is given, resident status. However, applying these types of criteria automatically excludes a large number of carers. The amount of time spent caring, the tasks performed, whether or not the carer lives with the care recipient are likely to vary, for example, between men and women or according to the carer's relationship to the care recipient.
As yet there is no clear or agreed definition of a carer in the literature. In this initial wave of data collection it was our intention to sample a comprehensive range of people providing differing levels and types of support to family members who, in turn, represented a range of disabling conditions. The study is based on the assumption that the impact of caregiving may vary significantly with relationship, gender, life stage, number of children, financial situation, employment, and so on. Thus, the broad spectrum of caregiving in the community was included to explore differences between groups, and to take account of different levels of caring intensity, the effects of these on caregivers, and how these compare with the caregiving responsibilities of the general population. Self-identification appeared to work well in providing a basis for a conceptual analysis of caring and a more explicit definition of a carer. This will form the subject of a subsequent paper.
This paper has been limited to some basic descriptive information about the caregivers identified in the first wave of data collection in the study. Further analyses, including a variety of measures relating to the socio-emotional aspects of the caring role, coping strategies, life satisfaction and so on, are yet to be undertaken, as are comparisons with our group of non- special needs caregivers.
Unlike most previous research in the area, the family caregivers interviewed in this first wave of data-gathering were identified from a random survey of Victorian households. Hence, they are likely to reflect (within the limits imposed by the relatively small sample size of 98) the population of Victorian caregivers in all its apparent diversity.
Carers were men and women, but mostly women. They ranged from the very young to the very old, but the middle aged predominated. They were mostly mothers, daughters or spouses, but some were fathers, sons, grandchildren, siblings, daughters- in-law or friends. They were mostly co- resident or caring for a relative who lived alone; for some, however, the person for whom they cared lived with others or in residential care. Some had been caring for only a few months but for most it was years, even decades. Carers differed, too, in the amount of time spent, the amount of help provided, and the tasks performed in caring for their relatives.
Not only was there heterogeneity in the carers but also in those for whom they cared: male and female, the very young through to the aged (but predominantly the latter). Most had multiple impairments, but the nature and severity of the illnesses and disabilities varied enormously. With the disability came a variety of difficult behaviours.
In spite of the demands of caring, use of formal services (other than medical) was very low. Carers relied mainly on family and friends for support. Even so, feelings of exhaustion prevailed and health problems in the carers themselves were not uncommon. Although paid employment was a welcome escape for some, the conflicting demands of work and caring commitments created problems. For those who were unable to take a job or were forced to work fewer hours or refuse promotion because of their caregiving role, the financial implications are obvious.
In conclusion, the pleasing response rate and the fact that almost all the carers interviewed agreed to be re-interviewed on subsequent occasions highlight the effectiveness of the CATI system for both identifying and interviewing family caregivers, as do the preliminary findings.
Clearly, with the diversity of caregiving roles and responses, a much larger sample of carers is required to, first, obtain an accurate profile of carers in the state, second, to explore, for example, the interactive effects of gender, residential status, relationship, nature of disability, age of carer and care recipient on the effects of caring, and, third and most importantly, to identify carer needs and strategies for easing the pressures.
APPENDIX
DEFINING 'CAREGIVERS'
In much past research, stringent criteria have been used for defining caregivers. For our purposes a carer could be a mother or a spouse providing 24 hours a day, seven days a week care, or a daughter, with her own family and work commitments, helping an aged parent with shopping, household chores for one hour on, say, four days a week.
Because the aim is to explore the impact of caregiving on family caregivers in a wide variety of circumstances and levels of intensity of care, caregivers were therefore selected on the basis of self-identification. The initial screening question asked whether the person had the main caring responsibility for someone who is aged or has a long-term illness, disability or other problems, even if they live elsewhere.
'Non-carers' were defined as people who were not caring for someone with special needs but who took primary responsibility for household tasks, including child care.
REFERENCES
- Bozic, S., (in preparation for publication), 'Carers in government policy: the case of the invisible and the invaluable', Department of Psychiatry, University of Melbourne.
- Braithwaite V. (1990), Bound to Care, Allen and Unwin, Sydney.
- Braithwaite V. (1992), 'Caregiving burden: making the concept scientifically useful and policy relevant, Research on Aging, 14 (1) pp.3-27.
- Brodaty H. and Gresham M. (1989), 'Effect of a training program to reduce stress in carers of patients with dementia', British Medical Journal, 299: pp.1375-1379.
- Draper, B.M., Poulos, C.J., Cole, A.M.D., Poulos, G.G. and Ehrlich, F. (1992), 'A comparison of caregivers for elderly stroke and dementia victims', Journal American Geriatric Society, 40: pp.896-901.
- Green, H. (1985), Informal Carers, General Household Survey, GHS No.15, Supplement A, HMSO, London.
- Herrman, H., Singh, B., Schofield, H., Eastwood, R., Burgess, P., Lewis, V. and Scotton, R., (in press), 'The health and wellbeing of informal caregivers: a review and study program', Australian Journal of Public Health.
- Hicks, N. (1991), 'Ageing Wellbeing and Research', Supplement to Australian Society, December.
- Levin, E., Sinclair, I. and Gorbach, P. (1989), Families, Services and Confusion in Old Age, Avebury, Hampshire.
- McCallum, J. (1992), 'Increasing longevity in Australia: autonomy versus health', Background paper prepared for the symposium, 'Longevity and Health in an Ageing Society', Melbourne.
- Mid-Term Review (1991), Aged Care Reform Strategy: Mid- Term Review, 1990-91, Commonwealth Department of Health, Housing and Community Services, AGPS, Canberra.
- Morris, R.G., Morris, L.W. and Britton, P.G. (1988), 'Factors affecting the emotional wellbeing of the caregivers of dementia sufferers', British Journal of Psychiatry , 153, pp.147-156.
- Murphy, B., Schofield, H. and Herrman H. (1992), 'Developments in the study of family caregiving: a review of caregiving instruments related to dementia', Paper prepared for the World Health Organization Project on Mental Health and Ageing, November.
- Otis, N. and Howe, A., 'Does Older Mean Sicker?', in Hicks N., 'Ageing, Wellbeing and Research', Supplement to Australian Society, December.
- Pearlin, L.I., Mullan, J.T., Semple, S.J., and Skaff, M.M. (1990), 'Caregiving and the stress process: an overview of concepts and their measures', The Gerontologist, 30 (5), pp.563-594.
- Raveis, V.H., Siegal, K. and Sudit, M. (1990), 'Psychological impact of caregiving on the care provider: a critical review of extant research', The Journal of Applied Social Sciences, 13 (1), pp.40-79.
- Rosenman, L. (1991), Community Care: Social or Economic Policy, SPRC National Social Policy Conference, University of NSW, July.
- Schultz, C.L. and Schultz, N.C. (1990), Caring for family caregivers, Australian Journal of Marriage and Family ,11, pp.84-93.